
上海交通大学学报(医学版) ›› 2026, Vol. 46 ›› Issue (3): 291-300.doi: 10.3969/j.issn.1674-8115.2026.03.003
• 论著 · 基础研究 • 上一篇
收稿日期:2025-11-04
接受日期:2025-12-10
出版日期:2026-03-28
发布日期:2026-03-30
通讯作者:
张绘莉,主任医师,博士;电子信箱:huilizhang815@163.com。基金资助:Received:2025-11-04
Accepted:2025-12-10
Online:2026-03-28
Published:2026-03-30
Contact:
Zhang Huili, E-mail: huilizhang815@163.com.Supported by:摘要:
目的·初步探究成纤维细胞线粒体功能障碍及其表型转化在肺动脉高压(pulmonary arterial hypertension,PAH)中的作用和机制。方法·采用野百合碱(monocrotaline,MCT)构建大鼠PAH模型。提取大鼠肺动脉外膜成纤维细胞(rat pulmonary arterial adventitial fibroblasts,RPAAFs),予以转化生长因子β1(transforming growth factor β1,TGF-β1)刺激构建成纤维细胞-肌成纤维细胞转化细胞模型。应用过氧化物酶体增殖物激活受体-γ共激活因子1α(peroxisome proliferator-activated receptor γ coactivator 1-α,Pgc1α)激动剂ZLN005以及线粒体质子载体解偶联剂Fccp进行干预。通过右心导管检测血流动力学指标,苏木精-伊红染色、免疫荧光染色评估肺血管重构情况。透射电镜和Mitotracker、TMRM和MitoSOX活细胞染色观察线粒体形态和功能。蛋白质印迹法检测Pgc1α、波形蛋白(vimentin)以及平滑肌肌动蛋白α(smooth muscle actin α,α-SMA)的表达水平,实时荧光定量PCR检测胶原蛋白Ⅰ型α1链(collagen type Ⅰ α 1,Col1a1)以及胶原蛋白Ⅲ型α1链(collagen type Ⅲ α 1,Col3a1)的mRNA表达水平。结果·MCT注射4周后,RPAAFs内线粒体碎片化,线粒体平均面积下降(P<0.001),Pgc1α蛋白的表达水平降低(P=0.016),促进成纤维细胞向肌成纤维细胞的转化。RPAAFs予以TGF-β1刺激后,细胞内线粒体数量减少(P<0.001)、膜电位降低(P=0.006)、活性氧升高(P<0.001),Pgc1α表达降低(P=0.006),α-SMA、Col1a1以及Col3a1表达显著升高(P=0.006)。RPAAFs给予Fccp刺激后,线粒体膜电位显著下降(P=0.005),α-SMA、Col1a1以及Col3a1表达同样显著升高(均P<0.001)。ZLN005预处理则上调Pgc1α的表达(P<0.001),改善TGF-β1诱导的线粒体功能障碍,并抑制TGF-β1诱导的成纤维细胞α-SMA的表达(P<0.001)。此外,ZLN005干预还可改善PAH大鼠的肺动脉重构,减轻血管周围胶原沉积,降低右心室收缩压和平均肺动脉压(均P<0.001),同时上调组织中Pgc1α表达并抑制α-SMA的表达(P=0.007)。结论·成纤维细胞线粒体功能障碍,促进成纤维细胞-肌成纤维细胞转化,在PAH的病理生理机制中发挥了重要作用。
中图分类号:
陈佳钰, 张绘莉. 成纤维细胞线粒体功能障碍在肺动脉高压中的作用和机制[J]. 上海交通大学学报(医学版), 2026, 46(3): 291-300.
Chen Jiayu, Zhang Huili. Role and mechanism of fibroblast mitochondrial dysfunction in pulmonary arterial hypertension[J]. Journal of Shanghai Jiao Tong University (Medical Science), 2026, 46(3): 291-300.
| Primer name | Sequences (5′→3′) |
|---|---|
| α-tubulin | |
| Forward | CTGATGTATGCCAAGCGTGC |
| Reverse | ATCCTTCTCTAGGGCAGCCA |
| Col1a1 | |
| Forward | CCAGCCGCAAAGAGTCTACAT |
| Reverse | ATGTCTTCTTGGCCATGCGT |
| Col3a1 | |
| Forward | GCCTACATGGATCAGGCCAA |
| Reverse | CATGGCCTTGCGTGTTTGAT |
表1 PCR引物序列
Tab 1 Primer sequences for PCR
| Primer name | Sequences (5′→3′) |
|---|---|
| α-tubulin | |
| Forward | CTGATGTATGCCAAGCGTGC |
| Reverse | ATCCTTCTCTAGGGCAGCCA |
| Col1a1 | |
| Forward | CCAGCCGCAAAGAGTCTACAT |
| Reverse | ATGTCTTCTTGGCCATGCGT |
| Col3a1 | |
| Forward | GCCTACATGGATCAGGCCAA |
| Reverse | CATGGCCTTGCGTGTTTGAT |
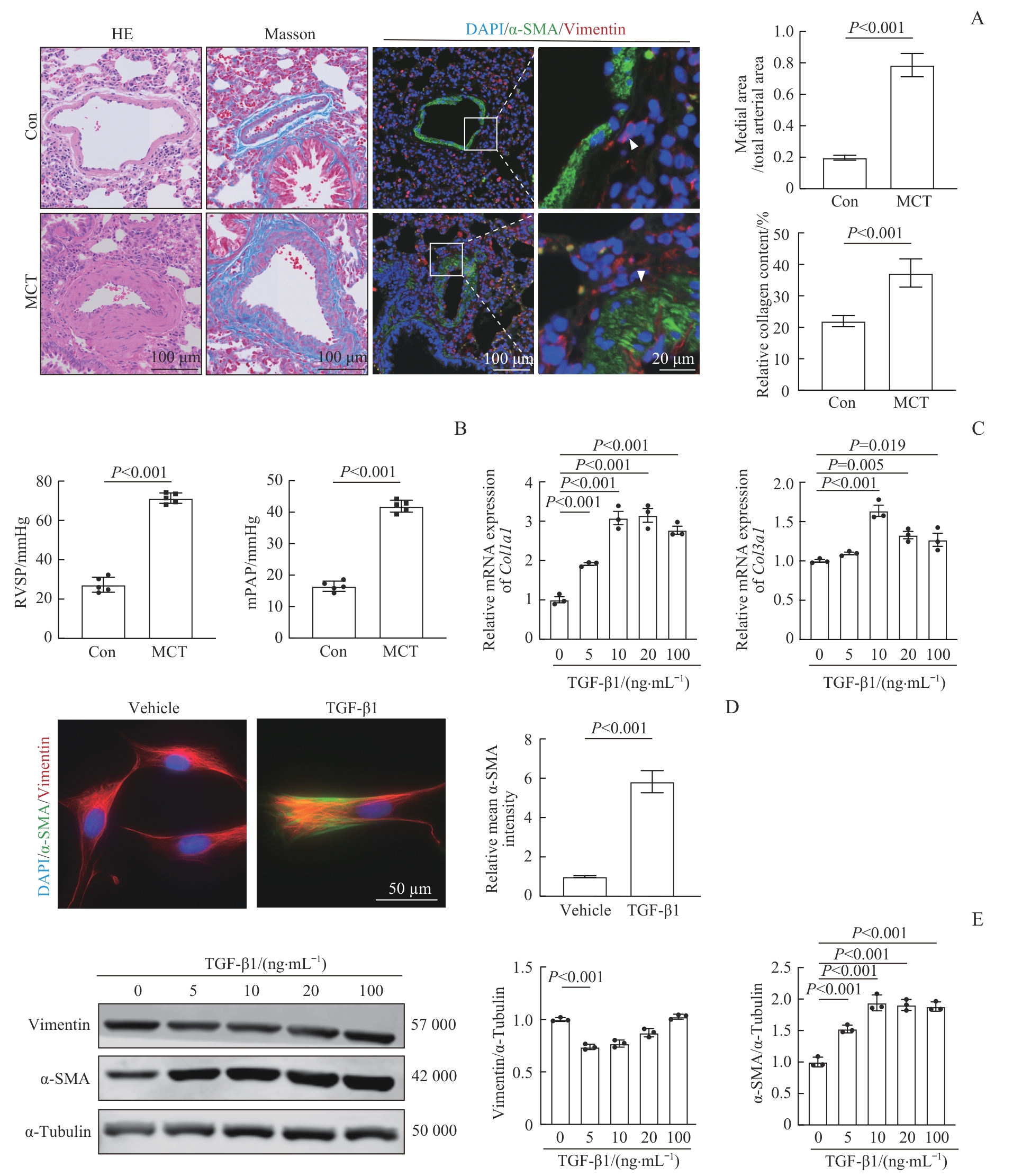
图1 PAH模型的建立以及成纤维细胞的FMTNote: A. Representative hematoxylin-eosin (HE) staining, Masson staining, and immunofluorescent staining images of rat pulmonary arteries. The ratio of medial area to total arterial area was used to assess vascular wall thickness, and the ratio of Masson-stained area to total arterial area was used to calculate the relative collagen content. B. RVSP and mPAP at 4 weeks after MCT treatment. 1 mmHg=0.133 kPa. C. Relative mRNA expression of Col1a1 and Col3a1 in RPAAFs. D. Immunofluorescent staining images of RPAAFs treated with vehicle or 10 ng/mL TGF-β1 for 24 h. E. Western blotting was performed to analyze the expression of vimentin, α-SMA, and α-tubulin in RPAAFs. Vimentin and α-SMA expression were normalized to α-tubulin.
Fig 1 Establishment of the PAH model and FMT in fibroblasts
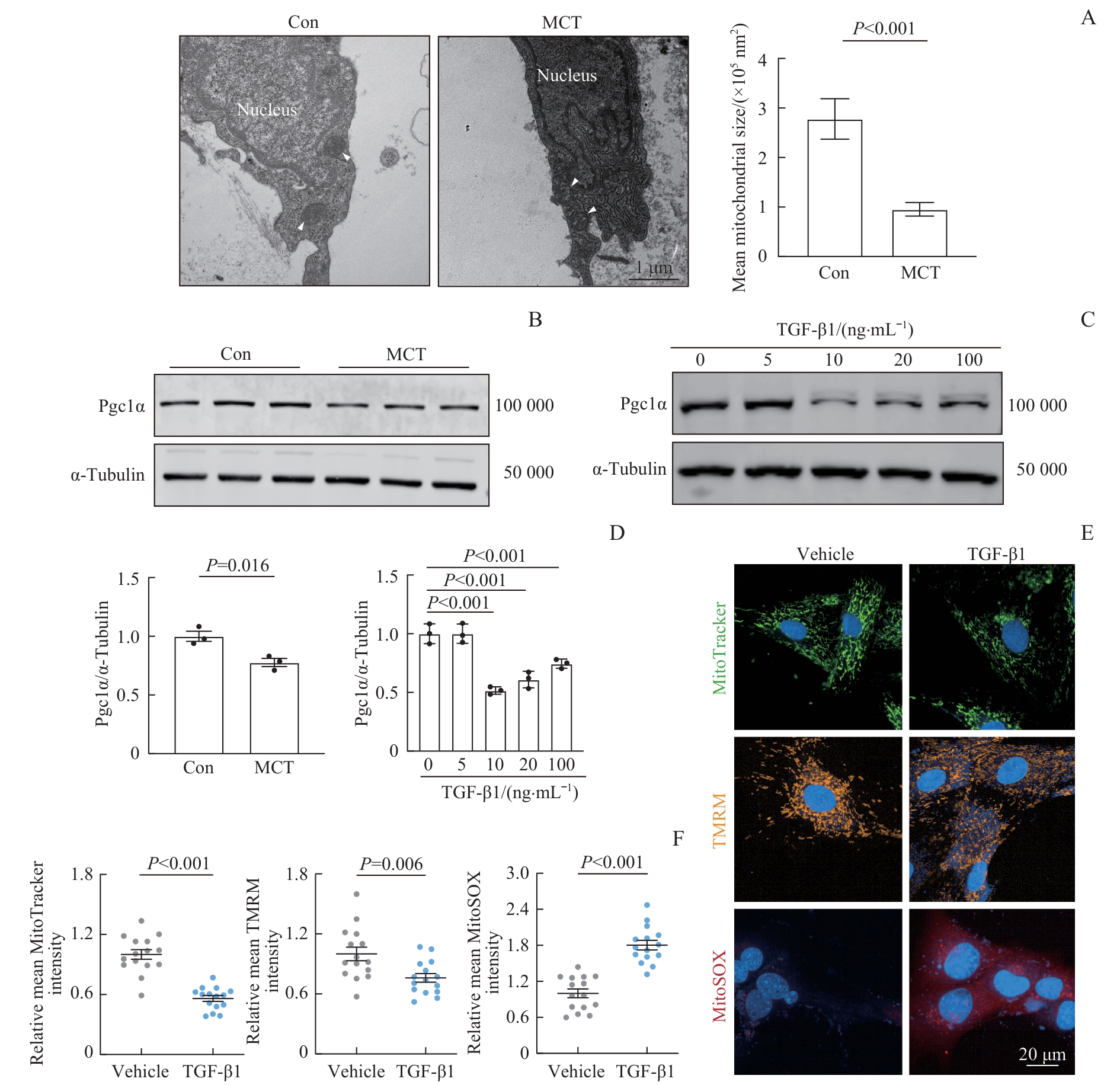
图2 PAH模型中成纤维细胞中的线粒体功能障碍Note: A. Transmission electron micrographs of pulmonary artery adventitial tissue, with quantification of mitochondria area per mitochondrion. B. Western blotting was performed to analyze Pgc1α expression in rat pulmonary artery adventitial tissue. C. Western blotting was performed to analyze Pgc1α expression in RPAAFs. D. Quantification of Pgc1α expression normalized to α-tubulin, summarizing data from panels B and C. E. Live-cell fluorescence imaging showing changes in mitochondrial mass (Mitotracker), mitochondrial membrane potential (TMRM), and oxidative stress exacerbation (MitoSOX) in RPAAFs treated with vehicle or 10 ng/mL TGF-β1 for 24 h. F. Quantification of relative mean fluorescence intensity per cell for Mitototracker, TMRM, and MitoSOX.
Fig 2 Mitochondrial dysfunction in fibroblasts in the PAH model
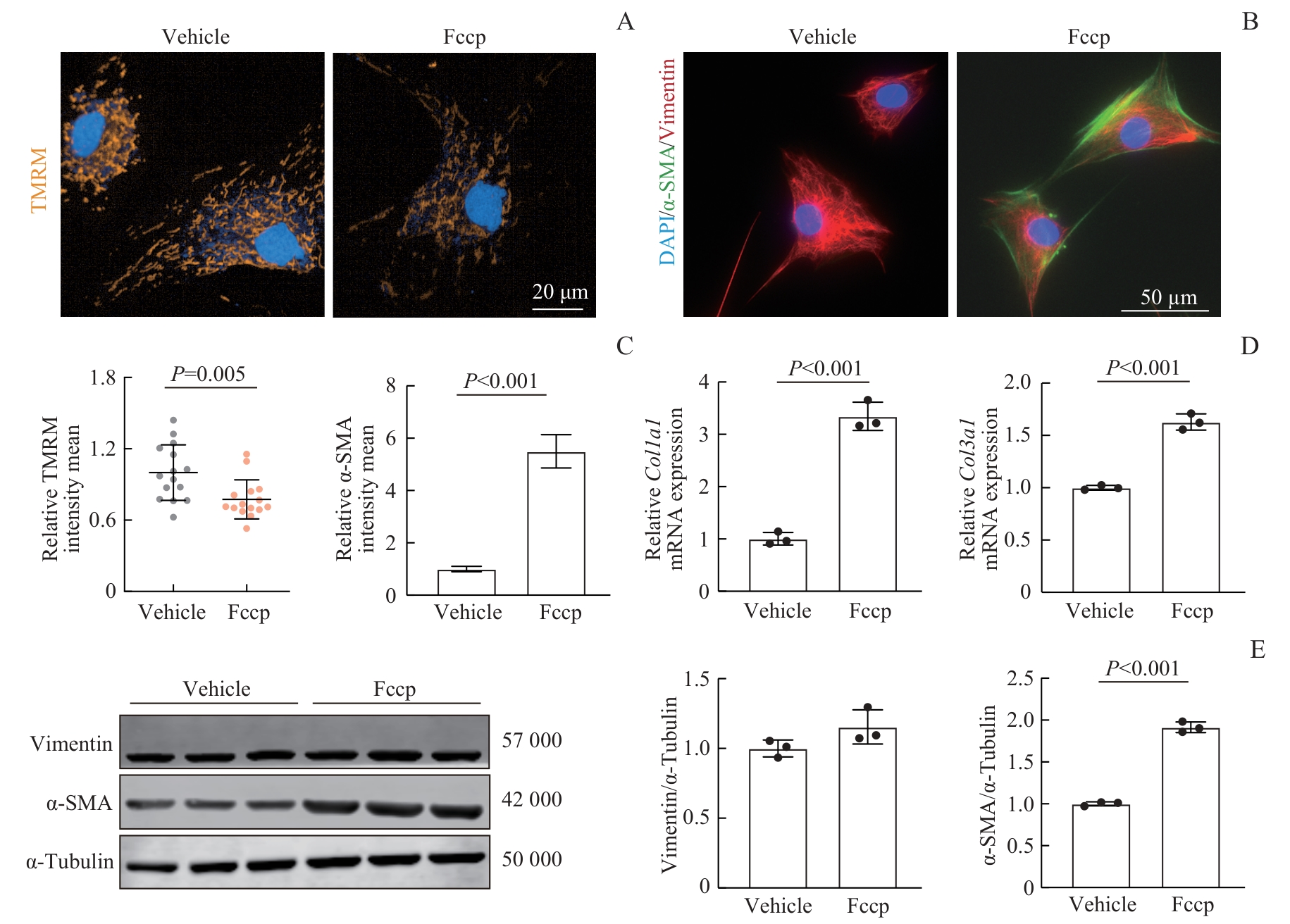
图3 Fccp介导的线粒体功能障碍及FMTNote: A. Live-cell fluorescence imaging showing changes in TMRM in fibroblasts under Fccp treatment. B. Immunofluorescent staining images of RPAAFs. C. Quantification of relative mean fluorescence intensity per cell for TMRM or α-SMA, summarizing data from panels A and B. D. Relative mRNA expression of Col1a1 and Col3a1 in RPAAFs. E. Western blotting was performed to detect the expression of vimentin, α-SMA, and α-tubulin in RPAAFs. Vimentin and α-SMA expression were normalized to α-tubulin.
Fig 3 Fccp-induced mitochondrial dysfunction and FMT
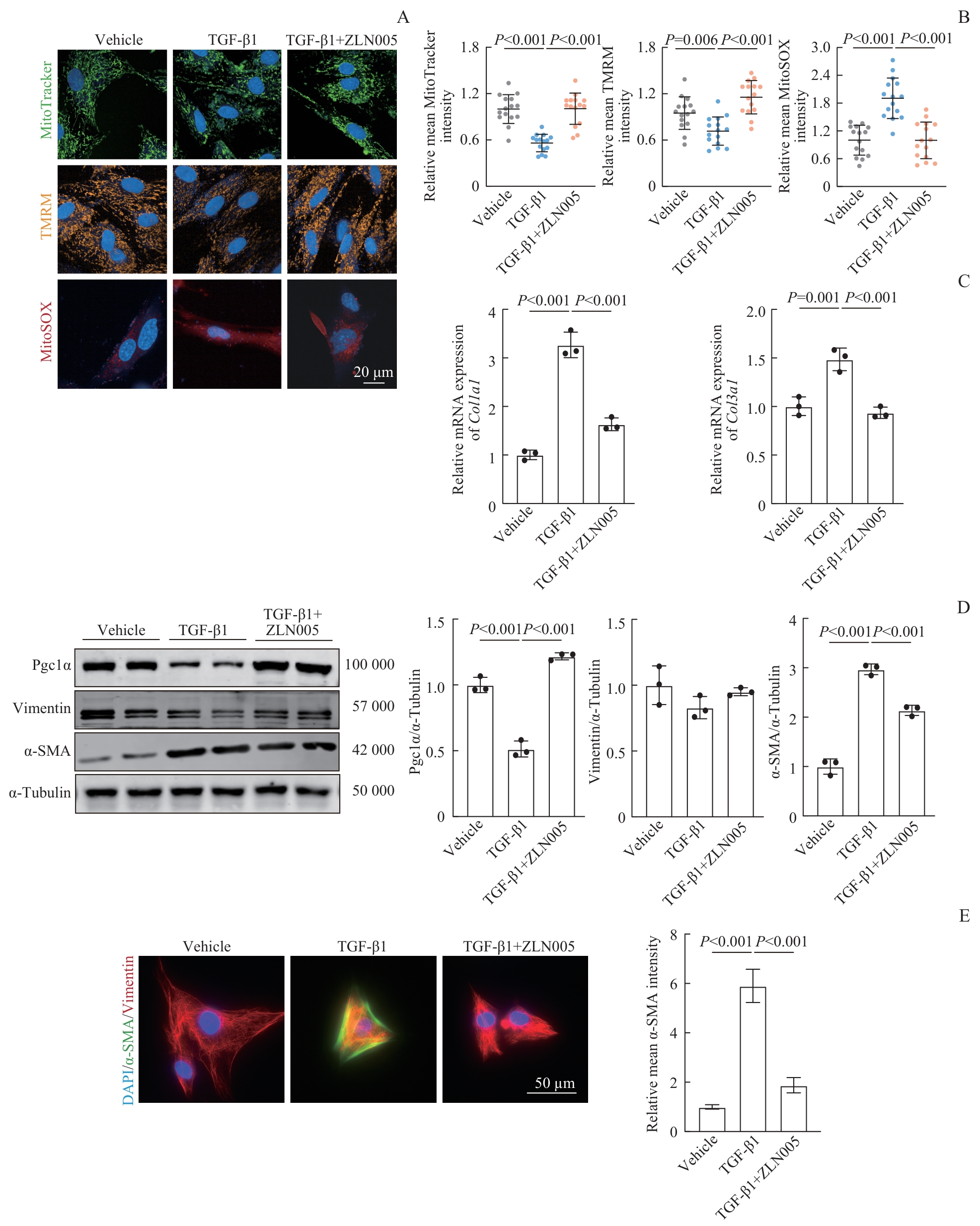
图4 ZLN005介导的线粒体功能改善以及FMT的抑制Note: A. Live-cell fluorescence imaging showing changes in Mitotracker, TMRM, and MitoSOX in fibroblast under TGF-β1 and ZLN005 treatment. B. Quantification of relative mean fluorescence intensity per cell for Mitototracker, TMRM, and MitoSOX. C. Relative mRNA expression of Col1a1 and Col3a1 in RPAAFs. D. Western blotting was performed to detect the expression of Pgc1α, vimentin, α-SMA, and α-tubulin in RPAAFs. Pgc1α, vimentin, and α-SMA expression were normalized to α-tubulin. E. Immunofluorescent (IF) staining images of RPAAFs and corresponding quantification.
Fig 4 ZLN005-mediated improvement in mitochondrial function and suppression of FMT
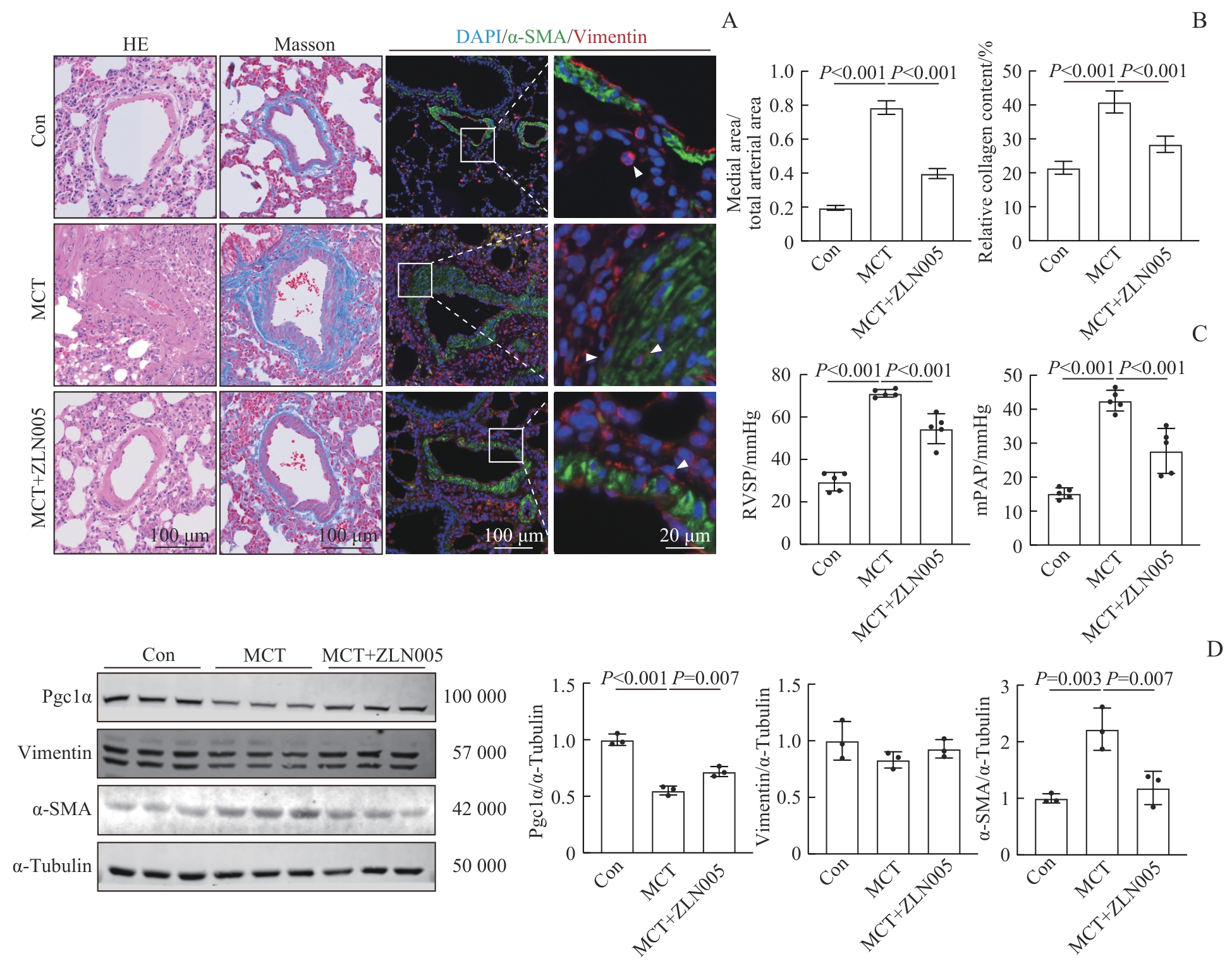
图5 ZLN005对大鼠PAH的改善Note: A. Representative hematoxylin-eosin (HE) staining, Masson staining, and immunofluorescent staining images of rat pulmonary arteries. B. The ratio of medial area to total arterial area was used to assess vascular wall thickness, and the ratio of Masson-stained area to total arterial area was used to calculate the relative collagen content. C. RVSP and mPAP at 4 weeks after MCT and ZLN005 treatment. D. Western blotting was performed to analyze the expression of Pgc1α, vimentin, α-SMA, and α-tubulin in rat pulmonary artery adventitial tissue. Pgc1α, vimentin, and α-SMA expression were normalized to α-tubulin.
Fig 5 Amelioration of PAH in rats induced by ZLN005
| [1] | Mocumbi A, Humbert M, Saxena A, et al. Pulmonary hypertension[J]. Nat Rev Dis Primers, 2024, 10: 1. |
| [2] | Strange G, Playford D, Stewart S, et al. Pulmonary hypertension: prevalence and mortality in the Armadale echocardiography cohort[J]. Heart, 2012, 98(24): 1805-1811. |
| [3] | Hassoun P M. Pulmonary arterial hypertension[J]. N Engl J Med, 2021, 385(25): 2361-2376. |
| [4] | Guignabert C, Aman J, Bonnet S, et al. Pathology and pathobiology of pulmonary hypertension: current insights and future directions[J]. Eur Respir J, 2024, 64(4): 2401095. |
| [5] | Thenappan T, Ormiston M L, Ryan J J, et al. Pulmonary arterial hypertension: pathogenesis and clinical management[J]. BMJ, 2018, 360: j5492. |
| [6] | Liang B H, Lin W C, Tang Y Y, et al. Selenium supplementation elevated SELENBP1 to inhibit fibroblast activation in pulmonary arterial hypertension[J]. iScience, 2024, 27(10): 111036. |
| [7] | Rachedi N S, Tang Y, Tai Y Y, et al. Dietary intake and glutamine-serine metabolism control pathologic vascular stiffness[J]. Cell Metab, 2024, 36(6): 1335-1350.e8. |
| [8] | Zhang H, Li M, Hu C J, et al. Fibroblasts in pulmonary hypertension: roles and molecular mechanisms[J]. Cells, 2024, 13(11): 914. |
| [9] | Kurose H. Cardiac fibrosis and fibroblasts[J]. Cells, 2021, 10(7): 1716. |
| [10] | Gibb A A, Lazaropoulos M P, Elrod J W. Myofibroblasts and fibrosis: mitochondrial and metabolic control of cellular differentiation[J]. Circ Res, 2020, 127(3): 427-447. |
| [11] | Seok B G, Lee S, Jin S H, et al. Inhibiting mitoNEET restores mitochondrial redox homeostasis and attenuates myofibroblast differentiation[J]. Free Radic Biol Med, 2025, 238: 293-302. |
| [12] | Halling J F, Pilegaard H. PGC-1α-mediated regulation of mitochondrial function and physiological implications[J]. Appl Physiol Nutr Metab, 2020, 45(9): 927-936. |
| [13] | Abu Shelbayeh O, Arroum T, Morris S, et al. PGC-1α is a master regulator of mitochondrial lifecycle and ROS stress response[J]. Antioxidants (Basel), 2023, 12(5): 1075. |
| [14] | Evans C E, Cober N D, Dai Z Y, et al. Endothelial cells in the pathogenesis of pulmonary arterial hypertension[J]. Eur Respir J, 2021, 58(3): 2003957. |
| [15] | Shen H, Gao Y, Ge D D, et al. BRCC3 regulation of ALK2 in vascular smooth muscle cells: implication in pulmonary hypertension[J]. Circulation, 2024, 150(2): 132-150. |
| [16] | MacKay C D A, Jadli A S, Fedak P W M, et al. Adventitial fibroblasts in aortic aneurysm: unraveling pathogenic contributions to vascular disease[J]. Diagnostics (Basel), 2022, 12(4): 871. |
| [17] | Younesi F S, Miller A E, Barker T H, et al. Fibroblast and myofibroblast activation in normal tissue repair and fibrosis[J]. Nat Rev Mol Cell Biol, 2024, 25(8): 617-638. |
| [18] | Wang A, Valdez-Jasso D. Cellular mechanosignaling in pulmonary arterial hypertension[J]. Biophys Rev, 2021, 13(5): 747-756. |
| [19] | Humbert M, Guignabert C, Bonnet S, et al. Pathology and pathobiology of pulmonary hypertension: state of the art and research perspectives[J]. Eur Respir J, 2019, 53(1): 1801887. |
| [20] | Wang D R, Zhang H, Li M, et al. microRNA-124 controls the proliferative, migratory, and inflammatory phenotype of pulmonary vascular fibroblasts[J]. Circ Res, 2014, 114(1): 67-78. |
| [21] | Chelladurai P, Boucherat O, Stenmark K, et al. Targeting histone acetylation in pulmonary hypertension and right ventricular hypertrophy[J]. Br J Pharmacol, 2021, 178(1): 54-71. |
| [22] | Khatun J, Gelles J D, Chipuk J E. Dynamic death decisions: how mitochondrial dynamics shape cellular commitment to apoptosis and ferroptosis[J]. Dev Cell, 2024, 59(19): 2549-2565. |
| [23] | Newmeyer D D, Ferguson-Miller S. Mitochondria: releasing power for life and unleashing the machineries of death[J]. Cell, 2003, 112(4): 481-490. |
| [24] | Su C T, See D H W, Huang Y J, et al. LTBP4 protects against renal fibrosis via mitochondrial and vascular impacts[J]. Circ Res, 2023, 133(1): 71-85. |
| [25] | Peng F, Liao M R, Jin W K, et al. 2-APQC, a small-molecule activator of Sirtuin-3 (SIRT3), alleviates myocardial hypertrophy and fibrosis by regulating mitochondrial homeostasis[J]. Signal Transduct Target Ther, 2024, 9(1): 133. |
| [26] | Ahangari F, Price N L, Malik S, et al. microRNA-33 deficiency in macrophages enhances autophagy, improves mitochondrial homeostasis, and protects against lung fibrosis[J]. JCI Insight, 2023, 8(4): e158100. |
| [27] | Zhang T, Liu C F, Zhang T N, et al. Overexpression of peroxisome proliferator-activated receptor γ coactivator 1-α protects cardiomyocytes from lipopolysaccharide-induced mitochondrial damage and apoptosis[J]. Inflammation, 2020, 43(5): 1806-1820. |
| [28] | Humeres C, Shinde A V, Tuleta I, et al. Fibroblast Smad7 induction protects the remodeling pressure-overloaded heart[J]. Circ Res, 2024, 135(3): 453-469. |
| [29] | Tie Y, Tang F, Peng D D, et al. TGF-beta signal transduction: biology, function and therapy for diseases[J]. Mol Biomed, 2022, 3(1): 45. |
| [30] | Kumar A P, Puthussery D T. Regulation of PPAR-γ coactivator-1α and its implication in mitochondrial function and neurodegenerative diseases[J]. Ageing Res Rev, 2025, 112: 102887. |
| [31] | Huang T, Zhang T Y, Gao J Q. Targeted mitochondrial delivery: a therapeutic new era for disease treatment[J]. J Control Release, 2022, 343: 89-106. |
| [32] | Tohme C, Haykal T, Yang R Q, et al. ZLN005, a PGC-1α activator, protects the liver against ischemia-reperfusion injury and the progression of hepatic metastases[J]. Cells, 2024, 13(17): 1448. |
| [33] | Zhu P F, Ma H J, Cui S C, et al. ZLN005 alleviates in vivo and in vitro renal fibrosis via PGC-1α-mediated mitochondrial homeostasis[J]. Pharmaceuticals (Basel), 2022, 15(4): 434. |
| [34] | Hsu C H, Roan J N, Fang S Y, et al. Transplantation of viable mitochondria improves right ventricular performance and pulmonary artery remodeling in rats with pulmonary arterial hypertension[J]. J Thorac Cardiovasc Surg, 2022, 163(5): e361-e373. |
| [35] | Gollihue J L, Patel S P, Eldahan K C, et al. Effects of mitochondrial transplantation on bioenergetics, cellular incorporation, and functional recovery after spinal cord injury[J]. J Neurotrauma, 2018, 35(15): 1800-1818. |
| [1] | 李景聪, 赵涵, 林巧雯, 孙宏翔, 苏冰, 伍宁波. FGF2对小鼠肠道间质细胞R-spondin 1表达的调控作用[J]. 上海交通大学学报(医学版), 2025, 45(8): 939-948. |
| [2] | 姜芊羽, 姚程程, 季萍, 王颖. HAMA水凝胶促进皮肤创面愈合的组织局部微环境特征[J]. 上海交通大学学报(医学版), 2025, 45(8): 969-980. |
| [3] | 范冰彬, 何玉虎. 线粒体自噬在动脉型肺动脉高压中作用的研究进展[J]. 上海交通大学学报(医学版), 2025, 45(12): 1654-1661. |
| [4] | 韩瑞, 吴倩, 刘丹, 程棣, 张盈, 倪嘉成, 康飘, 陈安然, 于淑洁, 方启晨, 李华婷. 超重肥胖青少年认知功能的改变及其与血清FGF21水平的关系[J]. 上海交通大学学报(医学版), 2024, 44(1): 87-97. |
| [5] | 刘铁鑫, 林俊卿, 郑宪友. 靶向亚细胞结构治疗脊髓损伤的研究进展[J]. 上海交通大学学报(医学版), 2023, 43(2): 230-236. |
| [6] | 张剑, 宋菲, 王西樵. 成纤维细胞的自噬性溶解死亡在增生性瘢痕消退过程中的作用[J]. 上海交通大学学报(医学版), 2022, 42(1): 44-50. |
| [7] | 周天浩, 辛肇晨, 杜少倩, 曹源, 许静轩, 劳曾红, 王红霞. 乳腺癌类器官共培养技术的建立和优化[J]. 上海交通大学学报(医学版), 2021, 41(8): 1017-1024. |
| [8] | 唐晓梦1, 2,任玉倩1,熊 熙1, 2,缪惠洁1,邵卢晶1, 2,崔 云1,张育才1, 2,王春霞1, 2. 成纤维细胞生长因子19预测儿童脓毒症合并胃肠功能障碍的临床价值[J]. 上海交通大学学报(医学版), 2020, 40(9): 1236-1242. |
| [9] | 赵伟光,刘志宏. 肿瘤相关成纤维细胞调控肿瘤免疫炎症微环境的研究进展[J]. 上海交通大学学报(医学版), 2020, 40(9): 1288-1293. |
| [10] | 马一飞,李玉峰,郭桂梅,朱亚菊,龚莹靓,董 瑜. 新型尿液标志物在紫癜性肾炎患儿中的水平变化[J]. 上海交通大学学报(医学版), 2020, 40(6): 841-846. |
| [11] | 项潇琼,罗丽颖,傅扬,顾青,唐敏. 血管内皮生长因子对体外培养的人 Tenon s囊成纤维细胞的 纤维化及其富含半胱氨酸的酸性分泌蛋白表达的作用[J]. 上海交通大学学报(医学版), 2019, 39(8): 866-. |
| [12] | 史永平1,原 博2. 脂肪干细胞对转化生长因子β1干预下真皮成纤维细胞致纤维化能力的同步影响[J]. 上海交通大学学报(医学版), 2019, 39(12): 1382-. |
| [13] | 奚 箐,郑捷新,王西樵. 增生性瘢痕中血管内皮功能障碍对成纤维细胞功能的影响[J]. 上海交通大学学报(医学版), 2019, 39(10): 1122-. |
| [14] | 耿燕来 1, 2,倪磊 1, 3,时国朝 1, 3. D-二聚体联合超声心动图及下肢血管超声在肺血栓栓塞症中的诊断价值[J]. 上海交通大学学报(医学版), 2018, 38(10): 1219-. |
| [15] | 胡艳阁,郝健,张迪,杨川峰,宋晨璐,方勇 . 溴结构域蛋白 4 特异性抑制剂 JQ-1 对人增生性瘢痕的影响[J]. 上海交通大学学报(医学版), 2017, 37(7): 924-. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||
