
上海交通大学学报(医学版) ›› 2026, Vol. 46 ›› Issue (2): 188-199.doi: 10.3969/j.issn.1674-8115.2026.02.007
• 论著 · 临床研究 • 上一篇
薛玥1,2, 徐健1,2,3,4,5( ), 江怡宁1,2,6, 郁珽1,2, 林燕芬3,4,6, 张怡静3,4,6, Luo Zhongcheng3,4,7
), 江怡宁1,2,6, 郁珽1,2, 林燕芬3,4,6, 张怡静3,4,6, Luo Zhongcheng3,4,7
收稿日期:2025-05-05
接受日期:2025-10-30
出版日期:2026-02-28
发布日期:2026-02-28
通讯作者:
徐 健,主任医师,博士;电子信箱:sonia0616@sjtu.edu.cn。基金资助:
Xue Yue1,2, Xu Jian1,2,3,4,5( ), Jiang Yining1,2,6, Yu Ting1,2, Lin Yanfen3,4,6, Zhang Yijing3,4,6, Luo Zhongcheng3,4,7
), Jiang Yining1,2,6, Yu Ting1,2, Lin Yanfen3,4,6, Zhang Yijing3,4,6, Luo Zhongcheng3,4,7
Received:2025-05-05
Accepted:2025-10-30
Online:2026-02-28
Published:2026-02-28
Contact:
XU Jian, E-mail: sonia0616@sjtu.edu.cn.Supported by:摘要:
目的·探讨妊娠期体质量增加(gestational weight gain,GWG)在母乳喂养持续时间与幼儿神经发育关联中的作用,并探讨育龄妇女维持母乳喂养的适宜的GWG水平。方法·利用2010—2012年在上海市开展的前瞻性出生队列,于孕中晚期招募后,随访到产后24~36个月,收集GWG、母乳喂养持续时间及相关混杂因素等信息。采用格赛尔婴幼儿发育量表的发育商和中国幼儿气质量表得分评估幼儿的神经认知行为发育。采用两段式线性回归,评估不同GWG分层(过多、不足/适宜)下母乳喂养时间与幼儿神经发育间关联的差异,以及GWG与母乳喂养持续时间之间的关系。结果·共纳入225对母婴对,平均母乳喂养时间为7.4个月。校正混杂因素后发现,GWG过多时,当母乳喂养<6个月时,母乳喂养时间与幼儿的语言的发育商水平呈正相关,与气质的趋避性和适应性得分呈负相关(均P<0.05);当母乳喂养≥6月时,相关性均不显著(喂养<6月与喂养≥6月比较,P对数似然比均<0.05)。而当GWG适宜或不足时,没有观察到关联的显著差异(喂养<6月与喂养≥6月比较,P对数似然比均≥0.05)。GWG≥17.5 kg时,随着GWG增加,母乳喂养持续时间明显缩短。结论·GWG对母乳喂养持续时间与幼儿神经发育水平间的关联存在潜在影响。GWG过多时,鼓励母乳喂养时间达到6个月或6个月内尽可能长,有利于促进婴幼儿的神经发育。GWG控制在17.5 kg以下,有助于产后更长时间的母乳喂养。
中图分类号:
薛玥, 徐健, 江怡宁, 郁珽, 林燕芬, 张怡静, Luo Zhongcheng. 妊娠期体质量增加在母乳喂养时间与幼儿神经行为发展关联中的作用[J]. 上海交通大学学报(医学版), 2026, 46(2): 188-199.
Xue Yue, Xu Jian, Jiang Yining, Yu Ting, Lin Yanfen, Zhang Yijing, Luo Zhongcheng. Role of gestational weight gain in the association between breastfeeding duration and toddler neurodevelopment[J]. Journal of Shanghai Jiao Tong University (Medical Science), 2026, 46(2): 188-199.
| Variable | Demographic characteristic | Breastfeeding duration/month | Unadjusted association with breastfeeding duration [β(95%CI)] |
|---|---|---|---|
| Per capita family income level/n(%) | |||
| <2 000 yuan/month | 12 (5.3) | 7.2±5.0 | Reference |
| 2 000‒4 999 yuan/month | 64 (28.4) | 7.2±5.2 | 0 (-2.9, 2.9) |
| 5 000‒10 000 yuan/month | 91 (40.4) | 7.4±4.8 | 0.2 (-2.7, 3.0) |
| >10 000 yuan/month | 58 (25.8) | 7.7±4.0 | 0.5 (-2.4, 3.4) |
| Maternal factor | |||
| Maternal age at enrollment/n(%) | |||
| <25 years | 19 (8.4) | 5.1±3.5 | Reference |
| ≥25 years and <30 years | 127 (56.4) | 7.2±4.5 | 2.1 (-0.1, 4.4) |
| ≥30 years | 79 (35.1) | 8.3±5.1 | 3.2 (0.9, 5.6)① |
| Maternal educational degree/n(%) | |||
| Junior middle school or lower | 15 (6.7) | 8.5±4.7 | Reference |
| Senior middle school | 20 (8.9) | 6.4±5.6 | -2.1 (-5.2, 1.0) |
| University or college level | 162 (72.0) | 7.2±4.6 | -1.4 (-3.8, 1.1) |
| Postgraduate level | 28 (12.4) | 8.7±4.1 | 0.1 (-2.8, 3.1) |
| Pre-pregnancy BMI/kg·m-2 | 22.1±2.9 | ‒ | 0 (-0.2, 0.2) |
| Pre-pregnancy BMI group/n(%) | |||
| Underweight | 17 (7.6) | 7.4±3.0 | Reference |
| Normal weight | 157 (69.8) | 7.6±4.8 | 0.9 (-1.5, 3.2) |
| Overweight | 40 (17.8) | 7.3±4.3 | 0.6 (-2.0, 3.3) |
| Obesity | 11 (4.9) | 5.7±6.9 | -1.0 (-4.5, 2.6) |
| GSI during pregnancy/score | 1.2±0.2 | ‒ | -1.1 (-4.0, 1.8) |
| GSI at around 30 months postpartum/score | 1.3±0.3 | ‒ | -1.2 (-3.2, 0.9) |
| Gestational weeks/week | 39.4±1.2 | ‒ | 0 (-0.5, 0.5) |
| Mode of delivery/n(%) | |||
| Vaginal | 76 (33.8) | 7.8±5.0 | Reference |
| Caesarean section with indications | 72 (32.0) | 7.7±4.1 | -0.1 (-1.6, 1.5) |
| Caesarean section without indications | 77 (34.2) | 6.7±4.9 | -1.1 (-2.6, 0.4) |
| Parity/n(%) | |||
| Primiparous | 214 (95.1) | 7.3±4.6 | Reference |
| Multiparous | 11 (4.9) | 8.3±7.0 | 1.0 (-2.0, 3.9) |
| GWG/kg | 15.0±4.7 | ‒ | -0.1 (-0.2, 0.1) |
| GWG group/n(%) | |||
| Appropriate/inadequate GWG | 92 (42.8) | 7.3±4.3 | Reference |
| Excessive GWG | 123 (57.2) | 7.5±5.0 | 0.3 (-1.0, 1.6) |
| Maternal daily working hours after maternity leave/n(%) | |||
| >8 h | 109 (48.7) | 6.9±4.2 | Reference |
| 5‒8 h | 90 (40.2) | 7.2±4.5 | 0.3 (-1.0, 1.6) |
| <5 h | 25 (11.2) | 10.0±6.5 | 3.1 (1.1, 5.2)② |
| Living with children per week/n(%) | |||
| 7 d | 166 (74.4) | 8.0±4.8 | Reference |
| ≤6 d | 57 (25.6) | 5.6±3.9 | -2.4 (-3.8, -1.0)③ |
| Offspring′s characteristic | |||
| Infant sex/n(%) | |||
| Boy | 99 (44.0) | 7.6±5.1 | Reference |
| Girl | 126 (56.0) | 7.2±4.4 | -0.4 (-1.6, 0.9) |
| Birth weight/kg | 3.5±0.4 | ‒ | 0 (0, 0) |
表1 受试者的人口学特征及其与母乳喂养持续时间的未校正混杂因素的关联
Tab 1 Demographic characteristics of the subjects and unadjusted associations with breastfeeding duration
| Variable | Demographic characteristic | Breastfeeding duration/month | Unadjusted association with breastfeeding duration [β(95%CI)] |
|---|---|---|---|
| Per capita family income level/n(%) | |||
| <2 000 yuan/month | 12 (5.3) | 7.2±5.0 | Reference |
| 2 000‒4 999 yuan/month | 64 (28.4) | 7.2±5.2 | 0 (-2.9, 2.9) |
| 5 000‒10 000 yuan/month | 91 (40.4) | 7.4±4.8 | 0.2 (-2.7, 3.0) |
| >10 000 yuan/month | 58 (25.8) | 7.7±4.0 | 0.5 (-2.4, 3.4) |
| Maternal factor | |||
| Maternal age at enrollment/n(%) | |||
| <25 years | 19 (8.4) | 5.1±3.5 | Reference |
| ≥25 years and <30 years | 127 (56.4) | 7.2±4.5 | 2.1 (-0.1, 4.4) |
| ≥30 years | 79 (35.1) | 8.3±5.1 | 3.2 (0.9, 5.6)① |
| Maternal educational degree/n(%) | |||
| Junior middle school or lower | 15 (6.7) | 8.5±4.7 | Reference |
| Senior middle school | 20 (8.9) | 6.4±5.6 | -2.1 (-5.2, 1.0) |
| University or college level | 162 (72.0) | 7.2±4.6 | -1.4 (-3.8, 1.1) |
| Postgraduate level | 28 (12.4) | 8.7±4.1 | 0.1 (-2.8, 3.1) |
| Pre-pregnancy BMI/kg·m-2 | 22.1±2.9 | ‒ | 0 (-0.2, 0.2) |
| Pre-pregnancy BMI group/n(%) | |||
| Underweight | 17 (7.6) | 7.4±3.0 | Reference |
| Normal weight | 157 (69.8) | 7.6±4.8 | 0.9 (-1.5, 3.2) |
| Overweight | 40 (17.8) | 7.3±4.3 | 0.6 (-2.0, 3.3) |
| Obesity | 11 (4.9) | 5.7±6.9 | -1.0 (-4.5, 2.6) |
| GSI during pregnancy/score | 1.2±0.2 | ‒ | -1.1 (-4.0, 1.8) |
| GSI at around 30 months postpartum/score | 1.3±0.3 | ‒ | -1.2 (-3.2, 0.9) |
| Gestational weeks/week | 39.4±1.2 | ‒ | 0 (-0.5, 0.5) |
| Mode of delivery/n(%) | |||
| Vaginal | 76 (33.8) | 7.8±5.0 | Reference |
| Caesarean section with indications | 72 (32.0) | 7.7±4.1 | -0.1 (-1.6, 1.5) |
| Caesarean section without indications | 77 (34.2) | 6.7±4.9 | -1.1 (-2.6, 0.4) |
| Parity/n(%) | |||
| Primiparous | 214 (95.1) | 7.3±4.6 | Reference |
| Multiparous | 11 (4.9) | 8.3±7.0 | 1.0 (-2.0, 3.9) |
| GWG/kg | 15.0±4.7 | ‒ | -0.1 (-0.2, 0.1) |
| GWG group/n(%) | |||
| Appropriate/inadequate GWG | 92 (42.8) | 7.3±4.3 | Reference |
| Excessive GWG | 123 (57.2) | 7.5±5.0 | 0.3 (-1.0, 1.6) |
| Maternal daily working hours after maternity leave/n(%) | |||
| >8 h | 109 (48.7) | 6.9±4.2 | Reference |
| 5‒8 h | 90 (40.2) | 7.2±4.5 | 0.3 (-1.0, 1.6) |
| <5 h | 25 (11.2) | 10.0±6.5 | 3.1 (1.1, 5.2)② |
| Living with children per week/n(%) | |||
| 7 d | 166 (74.4) | 8.0±4.8 | Reference |
| ≤6 d | 57 (25.6) | 5.6±3.9 | -2.4 (-3.8, -1.0)③ |
| Offspring′s characteristic | |||
| Infant sex/n(%) | |||
| Boy | 99 (44.0) | 7.6±5.1 | Reference |
| Girl | 126 (56.0) | 7.2±4.4 | -0.4 (-1.6, 0.9) |
| Birth weight/kg | 3.5±0.4 | ‒ | 0 (0, 0) |
| Schedule | x±s | Single linear regression | Piece-wise linear regression | Likelihood ratio test | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Breastfeeding<6 month | Breastfeeding≥6 month | ||||||||||
| β (95%CI) | P value | β (95%CI) | P value | β (95%CI) | P value | P value | |||||
| DQ of GDS | |||||||||||
| Gross motor | 106.8±12.0 | 0 (-0.4, 0.4) | 0.950 | 0.2 (-0.8, 1.1) | 0.733 | 0 (-0.6, 0.5) | 0.854 | 0.719 | |||
| Fine motor | 97.0±12.8 | 0 (-0.4, 0.5) | 0.872 | 0.4 (-0.7, 1.4) | 0.504 | -0.1 (-0.7, 0.5) | 0.748 | 0.492 | |||
| Adaptive | 113.4±9.9 | 0.1 (-0.2, 0.4) | 0.668 | 0.4 (-0.3, 1.2) | 0.273 | -0.1 (-0.5, 0.4) | 0.721 | 0.293 | |||
| Language | 112.8±14.8 | 0.3 (-0.2, 0.7) | 0.304 | 1.0 (-0.1, 2.2) | 0.082 | -0.1 (-0.7, 0.6) | 0.837 | 0.131 | |||
| Interpersonal | 104.4±12.5 | 0.2 (-0.1, 0.6) | 0.210 | 1.0 (0.1, 2.0) | 0.030 | -0.1 (-0.6, 0.4) | 0.779 | 0.059 | |||
| Temperament scores of CTTS | |||||||||||
| Activity level | 3.2±0.6 | 0 (0, 0) | 0.941 | 0 (-0.1, 0) | 0.186 | 0 (0, 0) | 0.372 | 0.140 | |||
| Biological rhythms | 2.6±0.6 | 0 (0, 0) | 0.799 | 0 (-0.1, 0) | 0.126 | 0 (0, 0) | 0.391 | 0.104 | |||
| Approach-withdrawal | 3.0±0.8 | 0 (-0.1, 0) | 0.026 | -0.1 (-0.1, 0) | 0.015 | 0 (0, 0) | 0.586 | 0.080 | |||
| Adaptability | 2.9±0.7 | 0 (-0.1, 0) | 0.009 | -0.1 (-0.1, 0) | 0.002 | 0 (0, 0) | 0.623 | 0.023 | |||
| Intensity of reaction | 3.9±0.6 | 0 (0, 0) | 0.281 | 0 (-0.1, 0) | 0.084 | 0 (0, 0) | 0.885 | 0.141 | |||
| Mood | 2.6±0.6 | 0 (0, 0) | 0.298 | 0 (-0.1, 0) | 0.636 | 0 (0, 0) | 0.462 | 0.955 | |||
| Persistence | 2.8±0.6 | 0 (0, 0) | 0.355 | 0 (-0.1, 0) | 0.267 | 0 (0, 0) | 0.882 | 0.402 | |||
| Attention | 3.8±0.6 | 0 (0, 0) | 0.478 | 0 (0, 0.1) | 0.779 | 0 (0, 0) | 0.594 | 0.992 | |||
| Sensitivity | 3.9±0.7 | 0 (0, 0) | 0.854 | 0 (-0.1, 0.1) | 0.833 | 0 (0, 0) | 0.970 | 0.877 | |||
表2 母乳喂养持续时间与幼儿神经行为发育关联的分析(校正混杂因素)
Tab 2 Adjusted associations between breastfeeding duration and toddlers' neurobehavioral development
| Schedule | x±s | Single linear regression | Piece-wise linear regression | Likelihood ratio test | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Breastfeeding<6 month | Breastfeeding≥6 month | ||||||||||
| β (95%CI) | P value | β (95%CI) | P value | β (95%CI) | P value | P value | |||||
| DQ of GDS | |||||||||||
| Gross motor | 106.8±12.0 | 0 (-0.4, 0.4) | 0.950 | 0.2 (-0.8, 1.1) | 0.733 | 0 (-0.6, 0.5) | 0.854 | 0.719 | |||
| Fine motor | 97.0±12.8 | 0 (-0.4, 0.5) | 0.872 | 0.4 (-0.7, 1.4) | 0.504 | -0.1 (-0.7, 0.5) | 0.748 | 0.492 | |||
| Adaptive | 113.4±9.9 | 0.1 (-0.2, 0.4) | 0.668 | 0.4 (-0.3, 1.2) | 0.273 | -0.1 (-0.5, 0.4) | 0.721 | 0.293 | |||
| Language | 112.8±14.8 | 0.3 (-0.2, 0.7) | 0.304 | 1.0 (-0.1, 2.2) | 0.082 | -0.1 (-0.7, 0.6) | 0.837 | 0.131 | |||
| Interpersonal | 104.4±12.5 | 0.2 (-0.1, 0.6) | 0.210 | 1.0 (0.1, 2.0) | 0.030 | -0.1 (-0.6, 0.4) | 0.779 | 0.059 | |||
| Temperament scores of CTTS | |||||||||||
| Activity level | 3.2±0.6 | 0 (0, 0) | 0.941 | 0 (-0.1, 0) | 0.186 | 0 (0, 0) | 0.372 | 0.140 | |||
| Biological rhythms | 2.6±0.6 | 0 (0, 0) | 0.799 | 0 (-0.1, 0) | 0.126 | 0 (0, 0) | 0.391 | 0.104 | |||
| Approach-withdrawal | 3.0±0.8 | 0 (-0.1, 0) | 0.026 | -0.1 (-0.1, 0) | 0.015 | 0 (0, 0) | 0.586 | 0.080 | |||
| Adaptability | 2.9±0.7 | 0 (-0.1, 0) | 0.009 | -0.1 (-0.1, 0) | 0.002 | 0 (0, 0) | 0.623 | 0.023 | |||
| Intensity of reaction | 3.9±0.6 | 0 (0, 0) | 0.281 | 0 (-0.1, 0) | 0.084 | 0 (0, 0) | 0.885 | 0.141 | |||
| Mood | 2.6±0.6 | 0 (0, 0) | 0.298 | 0 (-0.1, 0) | 0.636 | 0 (0, 0) | 0.462 | 0.955 | |||
| Persistence | 2.8±0.6 | 0 (0, 0) | 0.355 | 0 (-0.1, 0) | 0.267 | 0 (0, 0) | 0.882 | 0.402 | |||
| Attention | 3.8±0.6 | 0 (0, 0) | 0.478 | 0 (0, 0.1) | 0.779 | 0 (0, 0) | 0.594 | 0.992 | |||
| Sensitivity | 3.9±0.7 | 0 (0, 0) | 0.854 | 0 (-0.1, 0.1) | 0.833 | 0 (0, 0) | 0.970 | 0.877 | |||
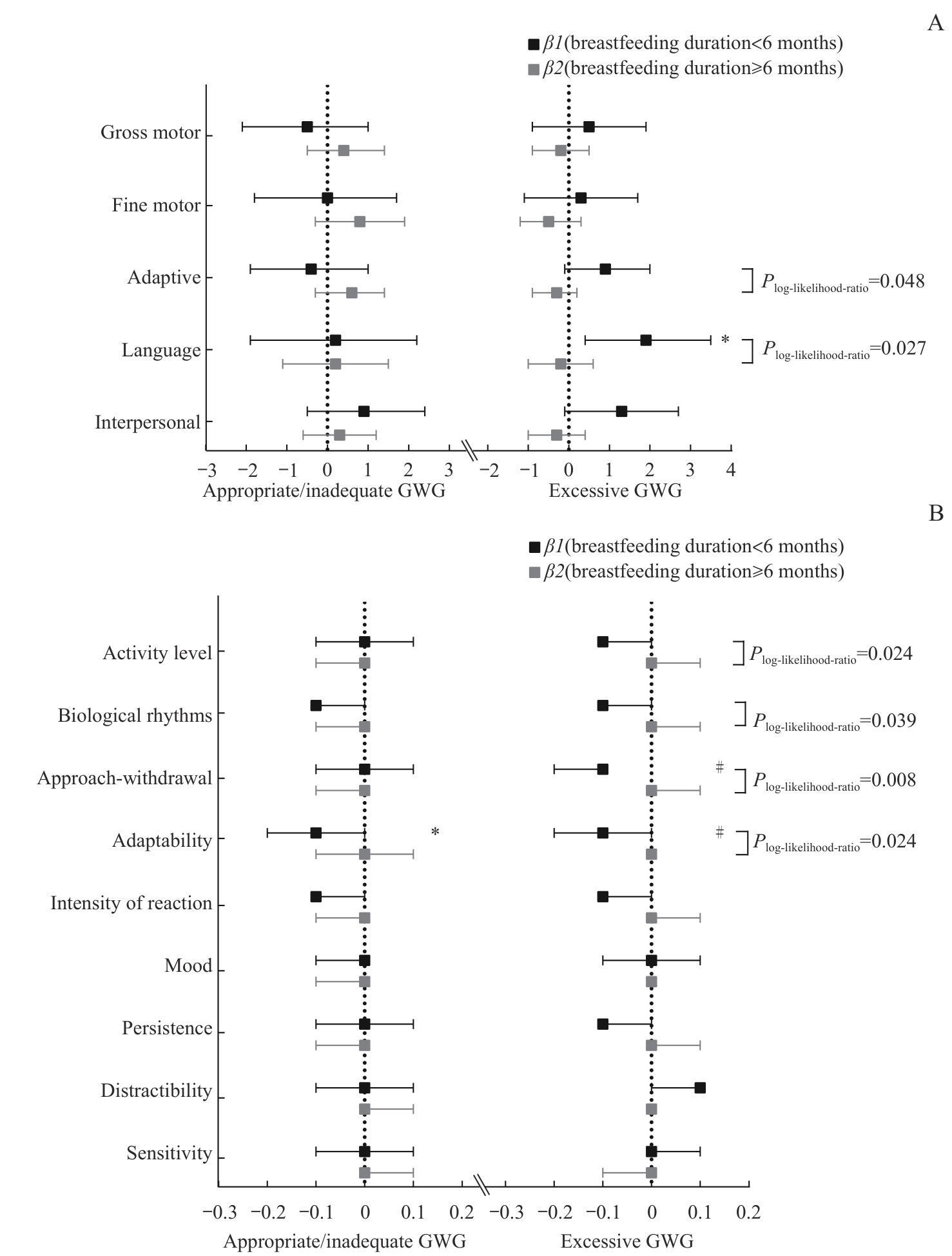
图1 基于CNS标准分析GWG分层下母乳喂养持续时间与幼儿神经行为发育关联的差异 [β(95%CI)]Note: A. Adjusted effects of breastfeeding duration on DQ of GDS. B. Adjusted effects of breastfeeding duration on scores of CTTS. Models were adjusted for maternal age, educational degree, per capita family income level, pre-pregnancy BMI, maternal prenatal stress, gestational age, birth weight at delivery, infant sex, infant age and feeding type. *P<0.05, #P<0.01.
Fig 1 Adjusted associations of breastfeeding duration with toddlers' neurobehavioral development under different GWG stratifications based on CNS guideline [β(95%CI)]
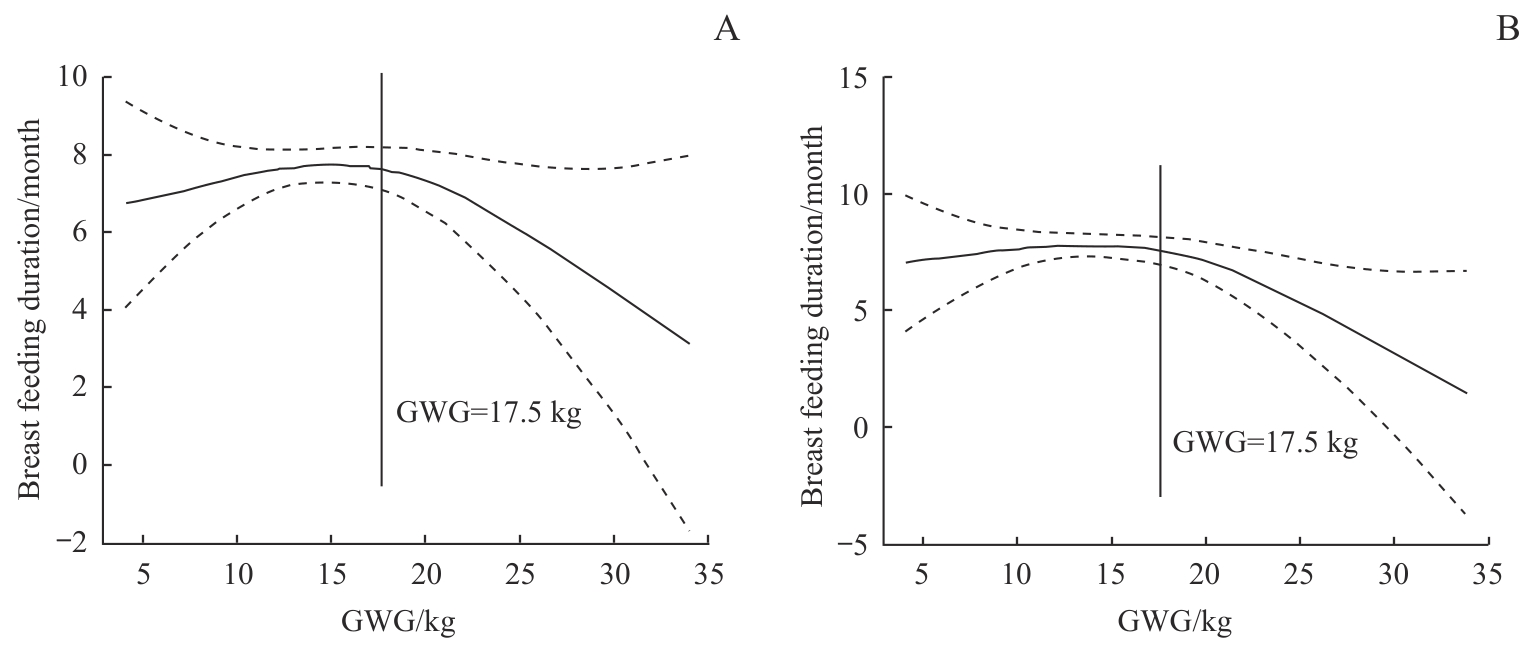
图2 母乳喂养持续时间随GWG的变化趋势Note: A. Unadjusted for confounding factors. B. Adjusted for confounding factors.
Fig 2 Trend of breastfeeding duration in relation to maternal GWG
| Regression | Unadjusted effect of GWG | Adjusted effect of GWG | |||
|---|---|---|---|---|---|
| β (95%CI) | P value | β (95%CI) | P value | ||
| Single linear regression | -0.1 (-0.2, 0.1) | 0.423 | -0.1 (-0.2, 0.1) | 0.397 | |
| Piece-wise linear regression | |||||
| β1 (GWG<17.5 kg) | 0.1 (-0.1, 0.4) | 0.222 | 0.1 (-0.1, 0.3) | 0.311 | |
| β2 (GWG≥17.5 kg) | -0.4 (-0.7, -0.1) | 0.019 | -0.4 (-0.7, -0.1) | 0.024 | |
| Likelihood ratio test P value | 0.026 | 0.026 | |||
表3 GWG与母乳喂养持续时间的关联
Tab 3 Associations of maternal GWG with breastfeeding duration
| Regression | Unadjusted effect of GWG | Adjusted effect of GWG | |||
|---|---|---|---|---|---|
| β (95%CI) | P value | β (95%CI) | P value | ||
| Single linear regression | -0.1 (-0.2, 0.1) | 0.423 | -0.1 (-0.2, 0.1) | 0.397 | |
| Piece-wise linear regression | |||||
| β1 (GWG<17.5 kg) | 0.1 (-0.1, 0.4) | 0.222 | 0.1 (-0.1, 0.3) | 0.311 | |
| β2 (GWG≥17.5 kg) | -0.4 (-0.7, -0.1) | 0.019 | -0.4 (-0.7, -0.1) | 0.024 | |
| Likelihood ratio test P value | 0.026 | 0.026 | |||
| [1] | Hauff L E, Leonard S A, Rasmussen K M. Associations of maternal obesity and psychosocial factors with breastfeeding intention, initiation, and duration[J]. Am J Clin Nutr, 2014, 99(3): 524-534. |
| [2] | Froń A, Orczyk-Pawiłowicz M. Breastfeeding beyond six months: evidence of child health benefits[J]. Nutrients, 2024, 16(22): 3891. |
| [3] | Rajagopalan V, Hsu E, Luo S. Breastfeeding duration and brain-body development in 9‒10-year-olds: modulating effect of socioeconomic levels[J]. Pediatr Res, 2025, 97(1): 378-386. |
| [4] | Lee H, Park H, Ha E, et al. Effect of breastfeeding duration on cognitive development in infants: 3-year follow-up study[J]. J Korean Med Sci, 2016, 31(4): 579-584. |
| [5] | Martinat M, Rossitto M, di Miceli M, et al. Perinatal dietary polyunsaturated fatty acids in brain development, role in neurodevelopmental disorders[J]. Nutrients, 2021, 13(4): 1185. |
| [6] | Fang X, Lee S, Rayalam S, et al. Docosahexaenoic acid supplementation and infant brain development: role of gut microbiome[J]. Nutr Res, 2024, 131: 1-13. |
| [7] | Chade E S, Júnior O R, Souza N M P, et al. The influence of nutritional status on brain development: benefits of exclusive breastfeeding[J]. Pediatr Rep, 2024, 16(3): 724-735. |
| [8] | 马佳妮, 崔巍, 张莺, 等. 产后6个月母乳喂养现况及影响因素的调查研究[J]. 中国计划生育学杂志, 2025, 33(2): 257-262. |
| Ma J N, Cui W, Zhang Y, et al. Investigation of the current status and the influencing factors of the breastfeeding of women within postpartum 6 months[J]. Chinese Journal of Family Planning, 2025, 33(2): 257-262. | |
| [9] | 张敏, 李晓乾, 幸玉华, 等. 渭南地区6月龄婴儿母乳喂养现状及影响因素调查[J]. 华南预防医学, 2023, 49(9): 1168-1170, 1175. |
| Zhang M, Li X Q, Xing Y H, et al. Status and influencing factors of breastfeeding for 6-month-old infants in Weinan region[J]. South China Journal of Preventive Medicine, 2023, 49(9): 1168-1170, 1175. | |
| [10] | 艾中华, 黄友, 朱翔龙, 等. 云南省0~5岁儿童母乳喂养持续时间及影响因素分析[J]. 昆明医科大学学报, 2024, 45(2): 112-116. |
| Ai Z H, Huang Y, Zhu X L, et al. Analysis of breastfeeding duration and influencing factors of children aged 0‒5 years in Yunnan Province[J]. Journal of Kunming Medical University, 2024, 45(2): 112-116. | |
| [11] | Derikonjic M, Vekic J, Stefanovic A, et al. Associations of excessive gestational weight gain with changes in components of maternal reverse cholesterol transport and neonatal outcomes[J]. Sci Rep, 2025, 15(1): 5716. |
| [12] | Zhang K D, Jia X M, Yu W J, et al. The associations of gestational weight gain and midpregnancy lipid levels with placental size and placental-to-birth weight ratio: findings from a Chinese birth cohort study[J]. BMC Pregnancy Childbirth, 2023, 23(1): 725. |
| [13] | Huang Y, Ouyang Y Q, Redding S R. Maternal prepregnancy body mass index, gestational weight gain, and cessation of breastfeeding: a systematic review and meta-analysis[J]. Breastfeed Med, 2019, 14(6): 366-374. |
| [14] | Dashti M, Scott J A, Edwards C A, et al. Predictors of breastfeeding duration among women in Kuwait: results of a prospective cohort study[J]. Nutrients, 2014, 6(2): 711-728. |
| [15] | Xiang M Y, Harbige L S, Zetterström R. Long-chain polyunsaturated fatty acids in Chinese and Swedish mothers: diet, breast milk and infant growth[J]. Acta Paediatr, 2005, 94(11): 1543-1549. |
| [16] | Ongprasert K, Ruangsuriya J, Malasao R, et al. Macronutrient, immunoglobulin A and total antioxidant capacity profiles of human milk from 1 to 24 months: a cross-sectional study in Thailand[J]. Int Breastfeed J, 2020, 15(1): 90. |
| [17] | Neves P A R, Gatica-Domínguez G, Santos I S, et al. Poor maternal nutritional status before and during pregnancy is associated with suspected child developmental delay in 2-year old Brazilian children[J]. Sci Rep, 2020, 10(1): 1851. |
| [18] | Fuemmeler B F, Zucker N, Sheng Y O, et al. Pre-pregnancy weight and symptoms of attention deficit hyperactivity disorder and executive functioning behaviors in preschool children[J]. Int J Environ Res Public Health, 2019, 16(4): 667. |
| [19] | Motoki N, Inaba Y, Shibazaki T, et al. Insufficient maternal gestational weight gain and infant neurodevelopment at 12 months of age: the Japan Environment and Children's Study[J]. Eur J Pediatr, 2022, 181(3): 921-931. |
| [20] | Jiang H L, Jia Y, Wang X Y, et al. Evaluating the application of the 2009 Institute of Medicine gestational weight gain guidelines on pregnant Chinese women[J]. Glob Health Action, 2023, 16(1): 2213494. |
| [21] | Gong X L, Wu T C, Zhang L Z, et al. Comparison of the 2009 Institute of Medicine and 2021 Chinese guidelines for gestational weight gain: a retrospective population-based cohort study[J]. Int J Gynecol Obstet, 2023, 162(3): 1033-1041. |
| [22] | Shan L, Feng J Y, Wang T T, et al. Prevalence and developmental profiles of autism spectrum disorders in children with global developmental delay[J]. Front Psychiatry, 2021, 12: 794238. |
| [23] | Gesell A,Amatruda C S. Developmental diagnosis: the evaluation and management of normal and abnormal neuropsychologic development in infancy and early childhood [M]. 3rd ed. Hagerstown, MD: Harper & Row, 1975. |
| [24] | Lin Y, Xu J, Huang J, et al. Effects of prenatal and postnatal maternal emotional stress on toddlers' cognitive and temperamental development [J]. J Affect Disord, 2017, 207: 9-17. |
| [25] | Zhu P, Sun M S, Hao J H, et al. Does prenatal maternal stress impair cognitive development and alter temperament characteristics in toddlers with healthy birth outcomes [J]. Dev Med Child Neurol, 2014, 56(3): 283-289. |
| [26] | Schauenburg H, Strack M. Measuring psychotherapeutic change with the symptom checklist SCL 90 R[J]. Psychother Psychosom, 1999, 68(4): 199-206. |
| [27] | Organization W H. Infant and young child feeding: model chapter for textbooks for medical students and allied health professionals[M]. Geneva: World Health Organization, 2008. |
| [28] | Institute of Medicine and National Research Council. Weight gain during pregnancy: reexamining the guidelines[M]. Washington DC:The National Academies Press, 2009. |
| [29] | Cai X D, Wardlaw T, Brown D W. Global trends in exclusive breastfeeding[J]. Int Breastfeed J, 2012, 7(1): 12. |
| [30] | de Lauzon-Guillain B, Thierry X, Bois C, et al. Maternity or parental leave and breastfeeding duration: results from the ELFE cohort[J]. Matern Child Nutr, 2019, 15(4): e12872. |
| [31] | Hamner H C, Chiang K V, Li R W. Returning to work and breastfeeding duration at 12 months, WIC infant and toddler feeding practices study-2[J]. Breastfeed Med, 2021, 16(12): 956-964. |
| [32] | Wu H H, Zhang Y Q, Zong X N, et al. Changes of feeding patterns in Chinese city children under 2 years from 1985 to 2015: results from a series of national cross-sectional surveys[J]. World J Pediatr, 2019, 15(2): 176-181. |
| [33] | Shao S S, Yan S Q, Zhu P, et al. Persistent pregnancy-related anxiety reduces breastfeeding exclusiveness and duration: a prospective cohort study[J]. Breastfeed Med, 2022, 17(7): 577-583. |
| [34] | Nurjanah S, Wirjatmadi B, Devy S R, et al. Predictors of breastfeeding duration on mothers who return to work: a systematic review[J]. J Public Health Afr, 2023, 14(2): 5. |
| [35] | Liu X X, Zhang J, Liu Y H, et al. The association between cesarean delivery on maternal request and method of newborn feeding in China[J]. PLoS One, 2012, 7(5): e37336. |
| [36] | Ulfa Y, Maruyama N, Igarashi Y, et al. Early initiation of breastfeeding up to six months among mothers after cesarean section or vaginal birth: a scoping review[J]. Heliyon, 2023, 9(6): e16235. |
| [37] | Cortés-Macías E, Selma-Royo M, Martínez-Costa C, et al. Breastfeeding practices influence the breast milk microbiota depending on pre-gestational maternal BMI and weight gain over pregnancy[J]. Nutrients, 2021, 13(5): 1518. |
| [38] | Jiang S J, Qin J L, Shi L, et al. Association among gestational weight gain, fucosylated human milk oligosaccharides, and breast milk microbiota: an evidence in healthy mothers from northwest China[J]. J Agric Food Chem, 2024, 72(45): 25135-25145. |
| [39] | Muhammad F, Fan B F, Wang R X, et al. The molecular gut-brain axis in early brain development[J]. Int J Mol Sci, 2022, 23(23): 15389. |
| [40] | Loh J S, Mak W Q, Tan L K S, et al. Microbiota-gut-brain axis and its therapeutic applications in neurodegenerative diseases[J]. Signal Transduct Target Ther, 2024, 9(1): 37. |
| [41] | Chen Y J, Xu J Y, Chen Y. Regulation of neurotransmitters by the gut microbiota and effects on cognition in neurological disorders[J]. Nutrients, 2021, 13(6): 2099. |
| [42] | Fan X X, Zang T Z, Liu J, et al. Changes in the gut microbiome in the first two years of life predicted the temperament in toddlers[J]. J Affect Disord, 2023, 333: 342-352. |
| [43] | Daiy K, Harries V, Nyhan K, et al. Maternal weight status and the composition of the human milk microbiome: a scoping review[J]. PLoS One, 2022, 17(10): e0274950. |
| [44] | Cohen Kadosh K, Muhardi L, Parikh P, et al. Nutritional support of neurodevelopment and cognitive function in infants and young children: an update and novel insights[J]. Nutrients, 2021, 13(1): 199. |
| [45] | Álvarez D, Muñoz Y, Ortiz M, et al. Impact of maternal obesity on the metabolism and bioavailability of polyunsaturated fatty acids during pregnancy and breastfeeding[J]. Nutrients, 2020, 13(1): 19. |
| [46] | de la Garza Puentes A, Martí Alemany A, Chisaguano A M, et al. The effect of maternal obesity on breast milk fatty acids and its association with infant growth and cognition: the PREOBE follow-up[J]. Nutrients, 2019, 11(9): 2154. |
| [47] | Khambadkone S G, Cordner Z A, Tamashiro K L K. Maternal stressors and the developmental origins of neuropsychiatric risk[J]. Front Neuroendocrinol, 2020, 57: 100834. |
| [48] | Cordner Z A, Khambadkone S G, Boersma G J, et al. Maternal high-fat diet results in cognitive impairment and hippocampal gene expression changes in rat offspring[J]. Exp Neurol, 2019, 318: 92-100. |
| [49] | Duthie L, Reynolds R M. Changes in the maternal hypothalamic-pituitary-adrenal axis in pregnancy and postpartum: influences on maternal and fetal outcomes[J]. Neuroendocrinology, 2013, 98(2): 106-115. |
| [50] | Feizabad M, Pourhabibi-Zarandi F, Barati-Boldaji R, et al. Association of maternal psychological distress and milk cortisol with infant temperament and growth[J]. Sci Rep, 2025, 15(1): 12885. |
| [51] | Natland S T, Andersen L F, Nilsen T I, et al. Maternal recall of breastfeeding duration twenty years after delivery[J]. BMC Med Res Methodol, 2012, 12: 179. |
| [52] | Scattolin M A A, Resegue R M, Rosário M C D. The impact of the environment on neurodevelopmental disorders in early childhood[J]. J Pediatr, 2022, 98(Suppl 1): S66-S72. |
| [53] | Zielinska-Pukos M A, Bryś J, Wesolowska A, et al. Breastmilk PUFA strongly associated with maternal dietary intake but not anthropometric parameters and breastmilk carotenoids[J]. Prostaglandins Leukot Essent Fatty Acids, 2022, 186: 102505. |
| [54] | Duan Y F, Yang Z Y, Lai J Q, et al. Exclusive breastfeeding rate and complementary feeding indicators in China: a national representative survey in 2013[J]. Nutrients, 2018, 10(2): 249. |
| [1] | 徐祖婧, 江怡宁, 徐健. 出生前母体重(类)金属复合暴露与子代认知和气质发育的相关性研究[J]. 上海交通大学学报(医学版), 2024, 44(12): 1570-1578. |
| [2] | 李燕, 江艳, 康琼芳, 陆群峰. 婴幼儿尿布性皮炎预防策略的最佳证据总结[J]. 上海交通大学学报(医学版), 2022, 42(3): 357-363. |
| [3] | 殷文, 王腾, 周雨曦, 杭燕南, 闻大翔. 婴幼儿活体肝移植术中静脉注射顺阿曲库铵的药效学研究[J]. 上海交通大学学报(医学版), 2021, 41(6): 761-763. |
| [4] | 董则含*,吴琰婷*,刘 含,王尹瑜,黄荷凤. 冰冻胚胎移植子代幼儿的体格和神经认知发育评估[J]. 上海交通大学学报(医学版), 2020, 40(6): 719-727. |
| [5] | 李彭举,钟 量,孙 杰. 输尿管软镜联合钬激光碎石术治疗婴幼儿上尿路结石:单中心32例研究[J]. 上海交通大学学报(医学版), 2020, 40(3): 408-. |
| [6] | 姜燕,李红云,朱昌娥,傅月珍,魏嵘. 气管导管外放置封堵支气管插管与单腔气管导管在婴幼儿单肺通气中的应用比较[J]. 上海交通大学学报(医学版), 2019, 39(5): 522-. |
| [7] | 石惠卿,王红兵,陈津津 . 上海市静安区12月龄婴儿丹佛发育筛查及其智能发育相关因素分析#br#[J]. 上海交通大学学报(医学版), 2017, 37(9): 1207-. |
| [8] | 姜磊,王伟,沈佳,张蔚,唐嘉忠,朱德明. 改进型体外循环管道在婴幼儿体外循环中的应用[J]. 上海交通大学学报(医学版), 2016, 36(4): 609-. |
| [9] | 苏杭,李质彬,杜江,江海峰,陈志康,孙海明,赵敏. 5年随访研究海洛因复吸的预测因子——气质、冲动性和COMT基因多态性的性别差异[J]. 上海交通大学学报(医学版), 2015, 35(10): 1452-. |
| [10] | 殷 文,闻大翔,杭燕南. 婴幼儿活体肝移植术中罗库溴铵持续输注的药效学研究[J]. 上海交通大学学报(医学版), 2014, 34(9): 1381-. |
| [11] | 朱 毓,万宏伟,黄 蓉. 产后6个月母乳喂养的护理干预进展[J]. 上海交通大学学报(医学版), 2013, 33(8): 1176-. |
| [12] | 朱瑜洁, 赵培泉, 张 琦. 129例永存原始玻璃体增生症的临床特征和术后疗效分析[J]. 上海交通大学学报(医学版), 2013, 33(6): 846-. |
| [13] | 孙 瑛, 朱 明, 张剑蔚, 等. 七氟醚预处理和后处理对婴幼儿体外循环心肌再灌注损伤的影响[J]. , 2011, 31(9): 1316-. |
| [14] | 朱亚菊, 林 芊, 华 丽, 等. 布地奈德混悬液联合妥洛特罗贴剂治疗婴幼儿反复喘息的疗效及安全性研究[J]. , 2011, 31(12): 1729-. |
| [15] | 苑成梅, 禹顺英, 李则挚, 等. 5-HTTLPR基因多态与双相障碍及其情感气质类型的关联研究[J]. , 2011, 31(11): 1518-. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||