
上海交通大学学报(医学版) ›› 2026, Vol. 46 ›› Issue (4): 529-536.doi: 10.3969/j.issn.1674-8115.2026.04.013
• 综述 • 上一篇
收稿日期:2025-07-02
接受日期:2025-08-22
出版日期:2026-04-28
发布日期:2026-04-28
通讯作者:
耿海霞,主任医师,硕士;电子信箱:haixia.geng@163.com。基金资助:
Liu Li1, Fan Haixia2, Geng Haixia3( )
)
Received:2025-07-02
Accepted:2025-08-22
Online:2026-04-28
Published:2026-04-28
Contact:
Geng Haixia, E-mail: haixia.geng@163.com.Supported by:摘要:
全球5%~12%的人口患有颞下颌关节紊乱病(temporomandibular disorders,TMD),该病可显著影响患者的口颌系统健康及生活质量。目前,针对该类患者的多学科管理方案尚缺乏共识,而近年来包含颞下颌关节科、正畸科和正颌外科在内的关节-颌骨-咬合联合诊治理念备受关注。功能性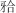 垫作为保守治疗的常用手段,对早中期TMD患者短期疗效显著,但长期稳定性仍待验证;颞下颌关节手术和正颌手术治疗可高效恢复中晚期TMD患者的颞下颌关节功能并纠正颌骨畸形,但正颌手术对颞下颌关节的影响需进一步研究。针对伴有(骨性)错
垫作为保守治疗的常用手段,对早中期TMD患者短期疗效显著,但长期稳定性仍待验证;颞下颌关节手术和正颌手术治疗可高效恢复中晚期TMD患者的颞下颌关节功能并纠正颌骨畸形,但正颌手术对颞下颌关节的影响需进一步研究。针对伴有(骨性)错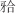 畸形的复杂TMD患者,关节-颌骨-咬合联合诊治通过多学科协同管理可实现个性化干预:功能性
畸形的复杂TMD患者,关节-颌骨-咬合联合诊治通过多学科协同管理可实现个性化干预:功能性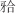 垫调整盘-髁关系、正畸治疗解除咬合干扰、手术治疗恢复关节与颌骨结构及功能;同时结合患者生长发育潜力制定个性化方案,争取以“最小创伤”促进关节-颌骨-咬合三维关系的长期稳定。该综述旨在为临床中TMD患者的多学科评估及个性化管理提供参考。
垫调整盘-髁关系、正畸治疗解除咬合干扰、手术治疗恢复关节与颌骨结构及功能;同时结合患者生长发育潜力制定个性化方案,争取以“最小创伤”促进关节-颌骨-咬合三维关系的长期稳定。该综述旨在为临床中TMD患者的多学科评估及个性化管理提供参考。
中图分类号:
刘莉, 范海霞, 耿海霞. 颞下颌关节紊乱病多学科联合诊治的临床研究进展[J]. 上海交通大学学报(医学版), 2026, 46(4): 529-536.
Liu Li, Fan Haixia, Geng Haixia. Clinical research progress in multidisciplinary collaborative diagnosis and treatment of temporomandibular disorders[J]. Journal of Shanghai Jiao Tong University (Medical Science), 2026, 46(4): 529-536.
| [1] | Shrivastava M, Battaglino R, Ye L. A comprehensive review on biomarkers associated with painful temporomandibular disorders[J]. Int J Oral Sci, 2021, 13(1): 23. |
| [2] | Klur T, Portegys S, Graf I, et al. Temporomandibular disorders: management of diagnostics and therapy in the context of orthodontic treatment: a survey among German orthodontists[J]. Dent J, 2025, 13(4): 167. |
| [3] | Wilkes C H. Internal derangements of the temporomandibular joint: pathological variations[J]. Arch Otolaryngol Head Neck Surg, 1989, 115(4): 469-477. |
| [4] | Shen P, Xie Q Y, Ma Z G, et al. Yang's classification of juvenile TMJ anterior disc displacement contributing to treatment protocols[J]. Sci Rep, 2019, 9(1): 5644. |
| [5] | Qin X Y, He Y Y, Zhang S Y, et al. Comparison of two different therapeutic approaches for skeletal class Ⅱ patients with temporomandibular degenerative joint disease[J]. Angle Orthod, 2023, 93(1): 49-56. |
| [6] | Myllymäki E, Heikinheimo K, Suominen A, et al. Longitudinal trends in temporomandibular joint disorder symptoms, the impact of malocclusion and orthodontic treatment: a 20-year prospective study[J]. J Oral Rehabil, 2023, 50(9): 739-745. |
| [7] | Al-Moraissi E A, Farea R, Qasem K A, et al. Effectiveness of occlusal splint therapy in the management of temporomandibular disorders: network meta-analysis of randomized controlled trials[J]. Int J Oral Maxillofac Surg, 2020, 49(8): 1042-1056. |
| [8] | Sun J L, Zhu H M, Lu C, et al. Temporomandibular joint disc repositioning and occlusal splint for adolescents with skeletal class Ⅱ malocclusion: a single-center, randomized, open-label trial[J]. BMC Oral Health, 2023, 23(1): 694. |
| [9] | Wroclawski C, Mediratta J K, Fillmore W J. Recent advances in temporomandibular joint surgery[J]. Medicina (Kaunas), 2023, 59(8): 1409. |
| [10] | Patel K, Eley K A, Cascarini L, et al. Temporomandibular disorders: review of evidence-based management and a proposed multidisciplinary care pathway[J]. Oral Surg Oral Med Oral Pathol Oral Radiol, 2023, 136(1): 54-69. |
| [11] | Dąbkowska I, Sobiech L, Czępińska A, et al. Multimodal approaches in the management of temporomandibular disorders: a narrative review[J]. J Clin Med, 2025, 14(12): 4326. |
| [12] | Korkmaz Y T, Altıntas N Y, Korkmaz F M, et al. Is hyaluronic acid injection effective for the treatment of temporomandibular joint disc displacement with reduction?[J]. J Oral Maxillofac Surg, 2016, 74(9): 1728-1740. |
| [13] | Derwich M, Pawlowska E. Do the mandibular condyles change their positions within glenoid fossae after occlusal splint therapy combined with physiotherapy in patients diagnosed with temporomandibular joint disorders? A prospective case control study[J]. J Pers Med, 2022, 12(2): 254. |
| [14] | Aidar L A, Abrahão M, Yamashita H K, et al. Herbst appliance therapy and temporomandibular joint disc position: a prospective longitudinal magnetic resonance imaging study[J]. Am J Orthod Dentofacial Orthop, 2006, 129(4): 486-496. |
| [15] | Güven B A, Ciğer S. Evaluation of the effect of fixed anterior biteplane treatment on temporomandibular joint in patients with deep bite[J]. Turk J Orthod, 2020, 33(1): 8-12. |
| [16] | Yildirim E, Karacay S, Erkan M. Condylar response to functional therapy with Twin-Block as shown by cone-beam computed tomography[J]. Angle Orthod, 2014, 84(6): 1018-1025. |
| [17] | Navaneetham A, Vaibhav N, Navaneetham R, et al. Efficacy of arthrocentesis and anterior repositioning splints in treatment of internal derangement of TMJ: a prospective clinical study[J]. Indian J Otolaryngol Head Neck Surg, 2023, 75(4): 3116-3129. |
| [18] | Shen P, Liu X H, Xie Q Y, et al. The effect evaluation of functional appliance used for class Ⅱ patients with temporomandibular joint anterior disc displacement[J]. J Craniofac Surg, 2019, 30(1): e15-e17. |
| [19] | Cheib Vilefort P L, Farah L O, Gontijo H P, et al. Condyle-glenoid fossa relationship after Herbst appliance treatment during two stages of craniofacial skeletal maturation: a retrospective study[J]. Orthod Craniofac Res, 2019, 22(4): 345-353. |
| [20] | Farouk K, Eissa O, Ghoneima A, et al. Treatment effects of Herbst appliance in skeletal class Ⅱ cases during pre-pubertal and post-pubertal periods: a cone-beam computed tomographic study[J]. Sci Rep, 2023, 13(1): 11342. |
| [21] | Halapanavar B, Padmini M N, Deshmukh S, et al. Comparison of skeletal changes in the temporomandibular joint between the twin block appliance and fixed functional appliance: a longitudinal follow-up study[J]. Int J Clin Pediatr Dent, 2024, 17(1): 7-14. |
| [22] | Ahmed M M S, Shi D L, Al-Somairi M A A, et al. Three dimensional evaluation of the skeletal and temporomandibular joint changes following stabilization splint therapy in patients with temporomandibular joint disorders and mandibular deviation: a retrospective study[J]. BMC Oral Health, 2023, 23(1): 18. |
| [23] | Kyburz K S, Eliades T, Papageorgiou S N. What effect does functional appliance treatment have on the temporomandibular joint? A systematic review with meta-analysis[J]. Prog Orthod, 2019, 20(1): 32. |
| [24] | Di Paolo C, Falisi G, Panti F, et al. "RA.DI.CA." splint for the management of the mandibular functional limitation: a retrospective study on patients with anterior disc displacement without reduction[J]. Int J Environ Res Public Health, 2020, 17(23): 9057. |
| [25] | Rabel K, Lüchtenborg J, Linke M, et al. 3D printed versus milled stabilization splints for the management of bruxism and temporomandibular disorders: study protocol for a randomized prospective single-blinded crossover trial[J]. Trials, 2024, 25(1): 589. |
| [26] | Musa M, Awad R, Izeldin S, et al. Quantitative and qualitative condylar changes following stabilization splint therapy in patients with temporomandibular joint disorders with and without skeletal lateral mandibular asymmetry: a cone beam computed tomographic study[J]. BMC Oral Health, 2024, 24(1): 363. |
| [27] | Bijelic T, Nilsson I M, List T, et al. Internet-based behavioural therapy for adolescents with temporomandibular disorder pain: a feasibility multicenter randomised controlled trial[J]. J Oral Rehabil, 2025, 52(9): 1275-1287. |
| [28] | Saglam R, Delilbasi C, Sayin Ozel G, et al. Evaluation of the effects of occlusal splint and masseter muscle injection in patients with myofascial pain: a randomised controlled trial[J]. J Oral Facial Pain Headache, 2024, 38(3): 64-76. |
| [29] | Zhang Y Y, Zheng J J, Wu Q Y, et al. Three-dimensional spatial analysis of temporomandibular joint in adolescent class Ⅱ division 1 malocclusion patients: comparison of Twin-Block and clear functional aligner[J]. Head Face Med, 2024, 20(1): 4. |
| [30] | Yilmaz O, Candirli C, Balaban E, et al. Evaluation of success criteria for temporomandibular joint arthrocentesis[J]. J Korean Assoc Oral Maxillofac Surg, 2019, 45(1): 15-20. |
| [31] | González L V, López J P, Díaz-Báez D, et al. Intraoperative complications in temporomandibular joint arthroscopy: a retrospective observational analysis of 899 arthroscopies[J]. J Craniomaxillofac Surg, 2022, 50(8): 651-656. |
| [32] | Ulmner M, Weiner C K, Lund B. Predictive factors in temporomandibular joint arthroscopy: a prospective cohort short-term outcome study[J]. Int J Oral Maxillofac Surg, 2020, 49(5): 614-620. |
| [33] | Jiao Z X, Wu S Y, Li J Y, et al. Imaging evaluation of disc position and status after temporomandibular joint arthroscopic disc repositioning and suturing surgery[J]. Heliyon, 2024, 10(4): e25526. |
| [34] | Chen B L, Qu X H. Surgical treatment of intracapsular temporomandibular disorders[J]. Acta Odontol Scand, 2024, 83: 273-280. |
| [35] | Dong H R, Lei J, Chen S, et al. The effect of disc repositioning on regenerative condylar bone remodelling in juvenile patients with temporomandibular joint osteoarthritis: a retrospective cohort study[J]. Clin Oral Investig, 2025, 29(2): 104. |
| [36] | Rauniyar D, Upadhyaya C, Chaurasia N, et al. Total temporomandibular joint replacement in recurrent temporomandibular joint ankylosis: a case report[J]. J Surg Case Rep, 2023, 2023(7): rjad426. |
| [37] | Almeida L E, Zammuto S, Mercuri L G. Quality of life outcomes following total temporomandibular joint replacement: a systematic review of long-term efficacy, functional improvements, and complication rates across prosthesis types[J]. J Clin Med, 2025, 14(14): 4859. |
| [38] | Murakami K, Yamamoto K, Kawakami M, et al. Changes in strain energy density in the temporomandibular joint disk after sagittal split ramus osteotomy using a computed tomography-based finite element model[J]. Fortschr Der Kieferorthopadie, 2024, 85(4): 289-305. |
| [39] | Castro V A, Pereira R M A, Mascarenhas G M, et al. Magnetic resonance imaging evaluation of articular disk position after orthognathic surgery with or without concomitant disk repositioning: a retrospective study[J]. Oral Surg Oral Med Oral Pathol Oral Radiol, 2021, 131(3): 276-285. |
| [40] | Kretschmer W B, Baciuţ G, Baciuţ M, et al. Effect of bimaxillary orthognathic surgery on dysfunction of the temporomandibular joint: a retrospective study of 500 consecutive cases[J]. Br J Oral Maxillofac Surg, 2019, 57(8): 734-739. |
| [41] | Kim H S, Han S S, Lee C. Unintentional temporomandibular joint disc reduction after orthognathic surgery: a case report with long-term imaging follow-up[J]. Imaging Sci Dent, 2022, 52(4): 409-413. |
| [42] | Aldayel A M, AlGahnem Z J, Alrashidi I S, et al. Orthodontics and temporomandibular disorders: an overview[J]. Cureus, 2023, 15(10): e47049. |
| [43] | Albagieh H, Alomran I, Binakresh A, et al. Occlusal splints-types and effectiveness in temporomandibular disorder management[J]. Saudi Dent J, 2023, 35(1): 70-79. |
| [44] | Demirovic K, Dzemidzic V, Nakas E. Impact of stabilization splint therapy on orthodontic diagnosis in patients with signs and symptoms of temporomandibular disorder[J]. Biomedicines, 2024, 12(10): 2251. |
| [45] | Shen P, Chen X W, Xie Q Y, et al. Assessment of occlusal appliance for the reposition of temporomandibular joint anterior disc displacement with reduction[J]. J Craniofacial Surg, 2019, 30(4): 1140-1143. |
| [46] | Kumar Maurya R, Singh H, Talwar B, et al. Biometric assessment of temporomandibular disorders in orthodontics: a multi-arm randomized controlled trial[J]. Turk J Orthod, 2022, 35(4): 290-306. |
| [47] | Amarista F J, Perez D E. Concomitant temporomandibular joint replacement and orthognathic surgery[J]. Diagnostics (Basel), 2023, 13(15): 2486. |
| [48] | Garcia M R, da Silva R D, Ferraz A X, et al. Prevalence of signs and symptoms related to temporomandibular disorders and orofacial pain in patients indicated for orthognathic surgery: a meta-analysis[J]. Clin Oral Investig, 2023, 27(7): 3307-3319. |
| [49] | Ueki K, Moroi A, Takayama A, et al. Assessment of temporomandibular joint disc position and skeletal stability after bimaxillary surgery[J]. Oral Maxillofac Surg, 2024, 28(1): 137-148. |
| [50] | Puthukkudiyil J S, Bhutia O, Roychoudhury A, et al. Does repositioning of temporomandibular joint disc with bone anchors provide better clinical outcomes than conventional disc plication procedures for anterior disc displacements without reduction in patients refractory to nonsurgical treatments?[J]. J Oral Maxillofac Surg, 2020, 78(12): 2160-2168. |
| [51] | Zhang P P, Ge Y H, Zhang J, et al. Orthodontic treatment improves magnetic resonance imaging features and quality of life in adult patients with temporomandibular disorders[J]. Am J Transl Res, 2023, 15(5): 3723-3730. |
| [52] | Khayat N, Winocur E, Kedem R, et al. The prevalence of temporomandibular disorders and dental attrition levels in patients with posterior crossbite and/or deep bite: a preliminary prospective study[J]. Pain Res Manag, 2021, 2021: 8827895. |
| [53] | Abate A, Cavagnetto D, Rusconi F M E, et al. Safety and effects of the rapid maxillary expander on temporomandibular joint in subjects affected by juvenile idiopathic arthritis: a retrospective study[J]. Children (Basel), 2021, 8(1): 33. |
| [54] | Zheng J J, Zhang Y Y, Wu Q Y, et al. Three-dimensional spatial analysis of the temporomandibular joint in adult patients with class Ⅱ division 2 malocclusion before and after orthodontic treatment: a retrospective study[J]. BMC Oral Health, 2023, 23(1): 477. |
| [55] | Huang Z W, Yang R, Gong C, et al. Treatment of severe open bite and mandibular condyle anterior displacement by mini-screws and four second molars extraction: a case report[J]. World J Clin Cases, 2023, 11(15): 3599-3611. |
| [56] | Dygas S, Szarmach I, Radej I. Assessment of the morphology and degenerative changes in the temporomandibular joint using CBCT according to the orthodontic approach: a scoping review[J]. Biomed Res Int, 2022, 2022: 6863014. |
| [57] | Perez D, Brown Z L, Amarista F J, et al. Treatment of malocclusion after TMJ disc repositioning with Mitek anchors. A retrospective review[J]. J Stomatol Oral Maxillofac Surg, 2019, 120(6): 540-544. |
| [58] | Zhu H M, He D M, Yang Z, et al. The effect of disc repositioning and post-operative functional splint for the treatment of anterior disc displacement in juvenile patients with class Ⅱ malocclusion[J]. J Craniomaxillofac Surg, 2019, 47(1): 66-72. |
| [59] | Fichera G, Ronsivalle V, Santonocito S, et al. Class Ⅱ skeletal malocclusion and prevalence of temporomandibular disorders. An epidemiological pilot study on growing subjects[J]. J Funct Morphol Kinesiol, 2021, 6(3): 63. |
| [60] | Lee Y C, Sohn H B, Park Y W, et al. Evaluation of postoperative changes in condylar positions after orthognathic surgery using balanced orthognathic surgery system[J]. Maxillofac Plast Reconstr Surg, 2022, 44(1): 11. |
| [61] | Schiavoni R, Contrafatto R, Grenga C, et al. Condylar reshaping in a TMD patient after ortho-prosthetic treatment: a 20-year follow-up case report[J]. J Clin Exp Dent, 2022, 14(2): e211-e216. |
| [62] | Shen P, Bai G, Xie Q Y, et al. Efficacy of arthroscopic diskopexy on condylar growth in temporomandibular joint anterior disk displacement: a randomized clinical trial[J]. Plast Reconstr Surg, 2024, 154(3): 544e-555e. |
| [63] | Sharma R, Muralidharan C G, Verma M, et al. MRI changes in the temporomandibular joint after mandibular advancement[J]. J Oral Maxillofac Surg, 2020, 78(5): 806-812. |
| [64] | Krarup H, Pedersen T K, Frid P, et al. Long-term follow-up of orthognathic surgery in 19 patients with juvenile idiopathic arthritis[J]. J Oral Maxillofac Res, 2023, 14(4): e4. |
| [65] | Nojima K, Nagata M, Ootake T, et al. Surgical orthodontic treatment involving mandibular premolar extraction in patient with mandibular retrusion associated with temporomandibular joint osteoarthritis[J]. Bull Tokyo Dent Coll, 2019, 60(2): 139-149. |
| [66] | Wang X H, Mao Y, Chen X Z, et al. Radiologic outcomes of temporomandibular joint disk repositioning by suturing through an open incision in adolescent patients with anterior disk displacement[J]. Oral Surg Oral Med Oral Pathol Oral Radiol, 2023, 135(5): 581-590. |
| [67] | Sato S, Kawamura H, Nagasaka H, et al. The natural course of anterior disc displacement without reduction in the temporomandibular joint: follow-up at 6, 12, and 18 months[J]. J Oral Maxillofac Surg, 1997, 55(3): 234-238. |
| [68] | Kurita K, Westesson P L, Yuasa H, et al. Natural course of untreated symptomatic temporomandibular joint disc displacement without reduction[J]. J Dent Res, 1998, 77(2): 361-365. |
| [1] | 孙磊, 戴世锋, 陈裕华, 许新怡, 姜克乐, 李筱文, 李承靖, 吴婷婷. 颞下颌关节紊乱病患者关节盘与髁突距离的定量分析研究[J]. 上海交通大学学报(医学版), 2025, 45(6): 684-692. |
| [2] | 孙一丹, 杨鑫. 焦虑增强颞下颌关节疼痛的脑功能磁共振成像研究[J]. 上海交通大学学报(医学版), 2025, 45(3): 342-348. |
| [3] | 杨海霞, 徐丽丽, 王博成, 陈敏洁. 磁共振引导的咀嚼肌疼痛放松训练疗效评估[J]. 上海交通大学学报(医学版), 2023, 43(5): 540-544. |
| [4] | 徐昱婷*,应王君子*,王舒泽,李 彪,王旭东. 上颌骨Le Fort Ⅰ型截骨前移后鼻唇部软组织变化的三维测量分析[J]. 上海交通大学学报(医学版), 2020, 40(6): 835-840. |
| [5] | 董晓晶 1,张男 1,甘露 1,吴怡颖 1,陈允允 1,方琼 2. 个案管理模式下老年乳腺癌患者辅助治疗依从性分析[J]. 上海交通大学学报(医学版), 2019, 39(2): 170-. |
| [6] | 虞 菲,陈思涵,于 倩,等. 抑郁症与颞下颌关节紊乱病关系的研究进展[J]. 上海交通大学学报(医学版), 2014, 34(10): 1548-. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||