
Journal of Shanghai Jiao Tong University (Medical Science) ›› 2024, Vol. 44 ›› Issue (1): 50-63.doi: 10.3969/j.issn.1674-8115.2024.01.006
• Clinical research • Previous Articles Next Articles
MA Jinqian1,2( ), FAN Pianpian1(
), FAN Pianpian1( ), ZHENG Tao1,3, ZHANG Lin3,4, CHEN Yuanzhi1, SHEN Jian5, OUYANG Fengxiu1,2(
), ZHENG Tao1,3, ZHANG Lin3,4, CHEN Yuanzhi1, SHEN Jian5, OUYANG Fengxiu1,2( )
)
Received:2023-06-09
Accepted:2023-12-05
Online:2024-01-28
Published:2024-02-28
Contact:
OUYANG Fengxiu
E-mail:mjq18335988098@126.com;447259743@qq.com;ouyangfengxiu@xinhuamed.com.cn
Supported by:CLC Number:
MA Jinqian, FAN Pianpian, ZHENG Tao, ZHANG Lin, CHEN Yuanzhi, SHEN Jian, OUYANG Fengxiu. Relationship among maternal gut, vaginal microbiota and microbiota in meconium and vernix caseosa in newborns[J]. Journal of Shanghai Jiao Tong University (Medical Science), 2024, 44(1): 50-63.
Add to citation manager EndNote|Ris|BibTeX
URL: https://xuebao.shsmu.edu.cn/EN/10.3969/j.issn.1674-8115.2024.01.006
| Characteristic | Value | Characteristic | Value |
|---|---|---|---|
| Maternal characteristic (n=11) | Weight gain in mid to late pregnancy/kg | 12.69±4.50 | |
| Age/year | 29.00±4.03 | Gestational diabetes mellitus/n(%) | 1(9.1) |
| Education level/n(%) | GBS positive/n(%) | 0(0) | |
| High school or below | 3(27.3) | Puerperal fever/n(%) | 0(0) |
| College or above | 8(72.7) | Infant characteristic (n=11) | |
| Parity/n(%) | Infant gender/n(%) | ||
| 0 | 8(72.7) | Girl | 4(36.4) |
| ≥1 | 3(27.3) | Boy | 7(63.6) |
| Antibiotics use during child delivery/n(%) | Weight for gestational age/n(%) | ||
| No | 8(72.7) | SGA | 2(18.2) |
| Yes | 3(27.3) | AGA | 8(72.7) |
| Early pregnancy BMI/n(%) | LGA | 1(9.1) | |
| <18.5 kg·m-2 | 0(0) | Entering NICU after birth/n(%) | |
| 18.5‒23.9 kg·m-2 | 8(72.7) | Yes | 1 (9.1) |
| 24.0‒27.9 kg·m-2 | 1(9.1) | No | 10(90.9) |
| ≥28 kg·m-2 | 2(18.2) | Gestational age at birth/week | 40.18±0.75 |
| Pre-delivery BMI/n(%) | Length/cm | 50.27±1.62 | |
| <18.5 kg·m-2 | 0(0) | Birth weight/g | 3 536.36±423.66 |
| 18.5‒23.9 kg·m-2 | 0(0) | Head circumference/cm | 34.55±1.21 |
| 24.0‒27.9 kg·m-2 | 6(54.5) | Birth BMI/(kg·m-2) | 13.96±1.15 |
| ≥28 kg·m-2 | 5(45.5) | Neonatal antibiotics use/n(%) | 0(0) |
Tab 1 Clinical characteristics of 11 pairs of mothers and newborns
| Characteristic | Value | Characteristic | Value |
|---|---|---|---|
| Maternal characteristic (n=11) | Weight gain in mid to late pregnancy/kg | 12.69±4.50 | |
| Age/year | 29.00±4.03 | Gestational diabetes mellitus/n(%) | 1(9.1) |
| Education level/n(%) | GBS positive/n(%) | 0(0) | |
| High school or below | 3(27.3) | Puerperal fever/n(%) | 0(0) |
| College or above | 8(72.7) | Infant characteristic (n=11) | |
| Parity/n(%) | Infant gender/n(%) | ||
| 0 | 8(72.7) | Girl | 4(36.4) |
| ≥1 | 3(27.3) | Boy | 7(63.6) |
| Antibiotics use during child delivery/n(%) | Weight for gestational age/n(%) | ||
| No | 8(72.7) | SGA | 2(18.2) |
| Yes | 3(27.3) | AGA | 8(72.7) |
| Early pregnancy BMI/n(%) | LGA | 1(9.1) | |
| <18.5 kg·m-2 | 0(0) | Entering NICU after birth/n(%) | |
| 18.5‒23.9 kg·m-2 | 8(72.7) | Yes | 1 (9.1) |
| 24.0‒27.9 kg·m-2 | 1(9.1) | No | 10(90.9) |
| ≥28 kg·m-2 | 2(18.2) | Gestational age at birth/week | 40.18±0.75 |
| Pre-delivery BMI/n(%) | Length/cm | 50.27±1.62 | |
| <18.5 kg·m-2 | 0(0) | Birth weight/g | 3 536.36±423.66 |
| 18.5‒23.9 kg·m-2 | 0(0) | Head circumference/cm | 34.55±1.21 |
| 24.0‒27.9 kg·m-2 | 6(54.5) | Birth BMI/(kg·m-2) | 13.96±1.15 |
| ≥28 kg·m-2 | 5(45.5) | Neonatal antibiotics use/n(%) | 0(0) |
| Characteristic | Value | Characteristic | Value |
|---|---|---|---|
| Maternal characteristic (n=14) | Weight gain in mid to late pregnancy/kg | 11.09±9.63 | |
| Age/year | 30.43±2.90 | Gestational diabetes mellitus/n(%) | 1(7.1) |
| Education level/n(%) | GBS positive/n(%) | 0(0) | |
| High school or below | 3(21.4) | Puerperal fever/n(%) | 0(0) |
| College or above | 11(78.6) | Infant characteristic (n=14) | |
| Parity/n(%) | Infant gender/n(%) | ||
| 0 | 10(71.4) | Girl | 7(50.0) |
| ≥1 | 4(28.6) | Boy | 7(50.0) |
| Antibiotics use during child delivery/n(%) | Weight for gestational age/n(%) | ||
| No | 11(78.57) | SGA | 0(0) |
| Yes | 3(21.43) | AGA | 10(71.4) |
| Early pregnancy BMI/n(%) | LGA | 4(28.6) | |
| <18.5 kg·m-2 | 0(0) | Entering NICU after birth/n(%) | |
| 18.5‒23.9 kg·m-2 | 11(78.6) | Yes | 2(14.3) |
| 24.0‒27.9 kg·m-2 | 2(14.3) | No | 12(85.7) |
| ≥28 kg·m-2 | 1(7.1) | Gestational age at birth/week | 39.14±0.95 |
| Pre-delivery BMI/n(%) | Length/cm | 50.00±0.88 | |
| <18.5 kg·m-2 | 0(0) | Birth weight/g | 3 418.93±371.51 |
| 18.5‒23.9 kg·m-2 | 2(14.3) | Birth BMI/(kg·m-2) | 13.66±1.26 |
| 24.0‒27.9 kg·m-2 | 8(57.1) | Neonatal antibiotics use/n(%) | 0(0) |
| ≥28 kg·m-2 | 4(28.6) | - | - |
Tab 2 Clinical characteristics of 14 newborns and their mothers
| Characteristic | Value | Characteristic | Value |
|---|---|---|---|
| Maternal characteristic (n=14) | Weight gain in mid to late pregnancy/kg | 11.09±9.63 | |
| Age/year | 30.43±2.90 | Gestational diabetes mellitus/n(%) | 1(7.1) |
| Education level/n(%) | GBS positive/n(%) | 0(0) | |
| High school or below | 3(21.4) | Puerperal fever/n(%) | 0(0) |
| College or above | 11(78.6) | Infant characteristic (n=14) | |
| Parity/n(%) | Infant gender/n(%) | ||
| 0 | 10(71.4) | Girl | 7(50.0) |
| ≥1 | 4(28.6) | Boy | 7(50.0) |
| Antibiotics use during child delivery/n(%) | Weight for gestational age/n(%) | ||
| No | 11(78.57) | SGA | 0(0) |
| Yes | 3(21.43) | AGA | 10(71.4) |
| Early pregnancy BMI/n(%) | LGA | 4(28.6) | |
| <18.5 kg·m-2 | 0(0) | Entering NICU after birth/n(%) | |
| 18.5‒23.9 kg·m-2 | 11(78.6) | Yes | 2(14.3) |
| 24.0‒27.9 kg·m-2 | 2(14.3) | No | 12(85.7) |
| ≥28 kg·m-2 | 1(7.1) | Gestational age at birth/week | 39.14±0.95 |
| Pre-delivery BMI/n(%) | Length/cm | 50.00±0.88 | |
| <18.5 kg·m-2 | 0(0) | Birth weight/g | 3 418.93±371.51 |
| 18.5‒23.9 kg·m-2 | 2(14.3) | Birth BMI/(kg·m-2) | 13.66±1.26 |
| 24.0‒27.9 kg·m-2 | 8(57.1) | Neonatal antibiotics use/n(%) | 0(0) |
| ≥28 kg·m-2 | 4(28.6) | - | - |

Fig 2 Box plots of Ace (A), Chao1 (B), Shannon (C), and Simpson (D) indices of maternal gut microbiota and vaginal microbiota in late-pregnancy and neonatal meconium microbiota
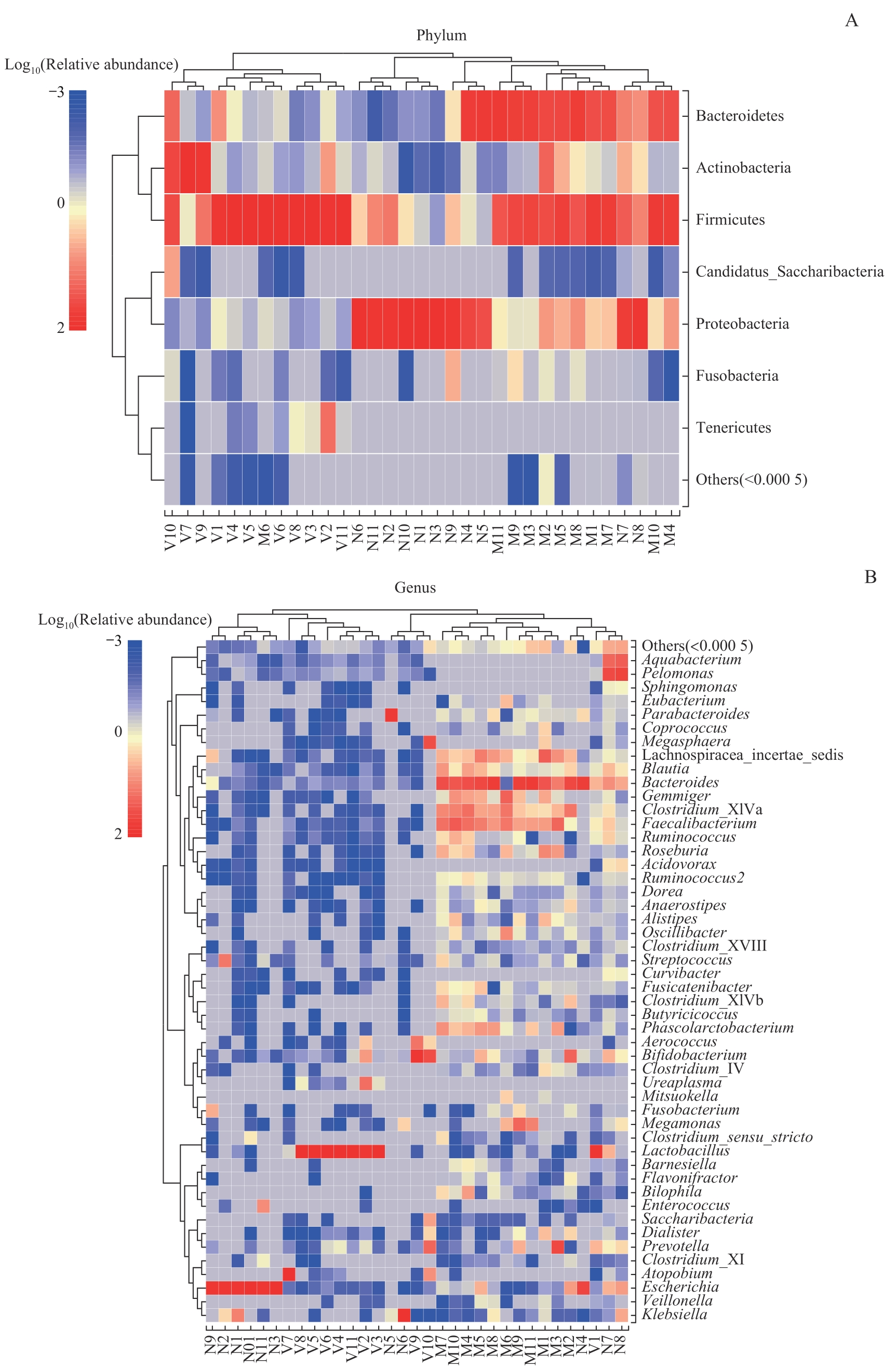
Fig 6 Species composition heatmaps at the level of phylum (A) and genus (B) in the maternal gut microbiota and maternal vaginal microbiota in late-pregnancy and neonatal meconium microbiota
| 1 | LI D T, WANG P, WANG P P, et al. The gut microbiota: a treasure for human health[J]. Biotechnol Adv, 2016, 34(7): 1210-1224. |
| 2 | WAMPACH L, HEINTZ-BUSCHART A, FRITZ J V, et al. Birth mode is associated with earliest strain-conferred gut microbiome functions and immunostimulatory potential[J]. Nat Commun, 2018, 9(1): 5091. |
| 3 | ARRIETA M C, ARÉVALO A, STIEMSMA L, et al. Associations between infant fungal and bacterial dysbiosis and childhood atopic wheeze in a nonindustrialized setting[J]. J Allergy Clin Immunol, 2018, 142(2): 424-434.e10. |
| 4 | RAUTAVA S, LUOTO R, SALMINEN S, et al. Microbial contact during pregnancy, intestinal colonization and human disease[J]. Nat Rev Gastroenterol Hepatol, 2012, 9(10): 565-576. |
| 5 | KRONMAN M P, ZAOUTIS T E, HAYNES K, et al. Antibiotic exposure and IBD development among children: a population-based cohort study[J]. Pediatrics, 2012, 130(4): e794-e803. |
| 6 | STOUT M J, CONLON B, LANDEAU M, et al. Identification of intracellular bacteria in the basal plate of the human placenta in term and preterm gestations[J]. Am J Obstet Gynecol, 2013, 208(3): 226.e1-226.e7. |
| 7 | MOREIRA L B, SILVA C B D, GERALDO-MARTINS V R, et al. Presence of Streptococcus mutans and interleukin-6 and -10 in amniotic fluid[J]. J Matern Fetal Neonatal Med, 2022, 35(25): 9463-9469. |
| 8 | WITT R G, BLAIR L, FRASCOLI M, et al. Detection of microbial cell-free DNA in maternal and umbilical cord plasma in patients with chorioamnionitis using next generation sequencing[J]. PLoS One, 2020, 15(4): e0231239. |
| 9 | MAKINO H, KUSHIRO A, ISHIKAWA E, et al. Mother-to-infant transmission of intestinal bifidobacterial strains has an impact on the early development of vaginally delivered infant's microbiota[J]. PLoS One, 2013, 8(11): e78331. |
| 10 | ARBOLEYA S, SÁNCHEZ B, MILANI C, et al. Intestinal microbiota development in preterm neonates and effect of perinatal antibiotics[J]. J Pediatr, 2015, 166(3): 538-544. |
| 11 | FALLANI M, YOUNG D, SCOTT J, et al. Intestinal microbiota of 6-week-old infants across Europe: geographic influence beyond delivery mode, breast-feeding, and antibiotics[J]. J Pediatr Gastroenterol Nutr, 2010, 51(1): 77-84. |
| 12 | VISSCHER M O, NARENDRAN V, PICKENS W L, et al. Vernix caseosa in neonatal adaptation[J]. J Perinatol, 2005, 25(7): 440-446. |
| 13 | ECHARRI P P, GRACIÁ C M, BERRUEZO G R, et al. Assessment of intestinal microbiota of full-term breast-fed infants from two different geographical locations[J]. Early Hum Dev, 2011, 87(7): 511-513. |
| 14 | TAPIAINEN T, PAALANNE N, TEJESVI M V, et al. Maternal influence on the fetal microbiome in a population-based study of the first-pass meconium[J]. Pediatr Res, 2018, 84(3): 371-379. |
| 15 | STINSON L F, BOYCE M C, PAYNE M S, et al. The not-so-sterile womb: evidence that the human fetus is exposed to bacteria prior to birth[J]. Front Microbiol, 2019, 10: 1124. |
| 16 | KLOPP J, FERRETTI P, MEYER C U, et al. Meconium microbiome of very preterm infants across Germany[J]. mSphere, 2022, 7(1): e0080821. |
| 17 | TANG N, LUO Z C, ZHANG L, et al. The association between gestational diabetes and microbiota in placenta and cord blood[J]. Front Endocrinol, 2020, 11: 550319. |
| 18 | MITCHELL C M, HAICK A, NKWOPARA E, et al. Colonization of the upper genital tract by vaginal bacterial species in nonpregnant women[J]. Am J Obstet Gynecol, 2015, 212(5): 611.e1-611.e9. |
| 19 | THEIS K R, ROMERO R, WINTERS A D, et al. Does the human placenta delivered at term have a microbiota? Results of cultivation, quantitative real-time PCR, 16S rRNA gene sequencing, and metagenomics[J]. Am J Obstet Gynecol, 2019, 220(3): 267.e1-267.e39. |
| 20 | STERPU I, FRANSSON E, HUGERTH L W, et al. No evidence for a placental microbiome in human pregnancies at term[J]. Am J Obstet Gynecol, 2021, 224(3): 296.e1-296.e23. |
| 21 | FERRETTI P, PASOLLI E, TETT A, et al. Mother-to-infant microbial transmission from different body sites shapes the developing infant gut microbiome[J]. Cell Host Microbe, 2018, 24(1): 133-145.e5. |
| 22 | ROBERTSON R C, MANGES A R, FINLAY B B, et al. The human microbiome and child growth: first 1000 days and beyond[J]. Trends Microbiol, 2019, 27(2): 131-147. |
| 23 | WAMPACH L, HEINTZ-BUSCHART A, HOGAN A, et al. Colonization and succession within the human gut microbiome by Archaea, bacteria, and microeukaryotes during the first year of life[J]. Front Microbiol, 2017, 8: 738. |
| 24 | MILLER J L, SONIES B C, MACEDONIA C. Emergence of oropharyngeal, laryngeal and swallowing activity in the developing fetal upper aerodigestive tract: an ultrasound evaluation[J]. Early Hum Dev, 2003, 71(1): 61-87. |
| 25 | MILANI C, DURANTI S, BOTTACINI F, et al. The first microbial colonizers of the human gut: composition, activities, and health implications of the infant gut microbiota[J]. Microbiol Mol Biol Rev, 2017, 81(4): e00036-e00017. |
| 26 | JIMÉNEZ E, FERNÁNDEZ L, MARÍN M L, et al. Isolation of commensal bacteria from umbilical cord blood of healthy neonates born by cesarean section[J]. Curr Microbiol, 2005, 51(4): 270-274. |
| 27 | LIU C J, LIANG X, NIU Z Y, et al. Is the delivery mode a critical factor for the microbial communities in the meconium?[J]. EBioMedicine, 2019, 49: 354-363. |
| 28 | GOMEZ DE AGÜERO M, GANAL-VONARBURG S C, FUHRER T, et al. The maternal microbiota drives early postnatal innate immune development[J]. Science, 2016, 351(6279): 1296-1302. |
| 29 | FERČEK I, LUGOVIĆ-MIHIĆ L, TAMBIĆ-ANDRAŠEVIĆ A, et al. Features of the skin microbiota in common inflammatory skin diseases[J]. Life, 2021, 11(9): 962. |
| 30 | TAÏEB A. Skin barrier in the neonate[J]. Pediatr Dermatol, 2018, 35(Suppl 1): s5-s9. |
| 31 | NISHIJIMA K, YONEDA M, HIRAI T, et al. Biology of the vernix caseosa: a review[J]. J Obstet Gynaecol Res, 2019, 45(11): 2145-2149. |
| 32 | MESFIN S, AFEWORK M, BIKILA D, et al. Distribution of vernix caseosa and associated factors among newborns delivered at Adama Comprehensive Specialized Hospital Medical College, Ethiopia, in 2022: cross-sectional study[J]. Clin Cosmet Investig Dermatol, 2022, 15: 2903-2914. |
| 33 | GRICE E A, KONG H H, CONLAN S, et al. Topographical and temporal diversity of the human skin microbiome[J]. Science, 2009, 324(5931): 1190-1192. |
| 34 | KONG H H. Skin microbiome: genomics-based insights into the diversity and role of skin microbes[J]. Trends Mol Med, 2011, 17(6): 320-328. |
| [1] | GAO Yu, YIN Shan, PANG Yue, LIANG Wenyi, LIU Yumin. Effect of rhubarb on gut microbiota-host co-metabolism in rats [J]. Journal of Shanghai Jiao Tong University (Medical Science), 2023, 43(8): 997-1007. |
| [2] | WEN Yajin, HE Wen, HAN Xiao, ZHANG Xiaobo. Exploratory analysis of gut microbiota differences in childhood asthma with different severity [J]. Journal of Shanghai Jiao Tong University (Medical Science), 2023, 43(6): 655-664. |
| [3] | WANG Jie, WU Hui, LU Lingpeng, YANG Kefeng, ZHU Jie, ZHOU Hengyi, YAO Die, GAO Ya, FENG Yuting, LIU Yuhong, JIA Jie. Dynamic changes in gut microbiota of women with gestational diabetes mellitus and the correlation with blood glucose, blood lipid and diet [J]. Journal of Shanghai Jiao Tong University (Medical Science), 2022, 42(9): 1336-1346. |
| [4] | LU Yu, WANG Hao, BA Qian. Role of gut microbiota in hepatocellular carcinoma: cancer occurrence, progresses and treatments [J]. Journal of Shanghai Jiao Tong University (Medical Science), 2022, 42(7): 939-944. |
| [5] | LI Yahui, WANG Yiwen, XIE Lijuan. A case of neonatal MIRAGE syndrome caused by novel mutation of SAMD9 gene [J]. Journal of Shanghai Jiao Tong University (Medical Science), 2022, 42(11): 1644-1648. |
| [6] | JIANG Yi, JIANG Ping, ZHANG Mingming, FANG Jingyuan. Research progress in the role of Akkermansia muciniphila in gut-related diseases [J]. Journal of Shanghai Jiao Tong University (Medical Science), 2022, 42(10): 1490-1497. |
| [7] | Ying-dan ZHANG, Zhen WANG. Research progress of the role of gut microbiota in the pathogenesis and treatment of obsessive-compulsive disorder [J]. JOURNAL OF SHANGHAI JIAOTONG UNIVERSITY (MEDICAL SCIENCE), 2021, 41(7): 967-971. |
| [8] | CHU Wei-wei, XU Jie-ying, LI Shang, ZHAI Jun-yu, DU Yan-zhi. Gut microbiota of polycystic ovary syndrome model rats induced with dehydroepiandrosterone [J]. , 2019, 39(9): 975-. |
| [9] | DENG Di, ZHAO Min. Research progress of gut microbiota in substance dependence [J]. , 2019, 39(3): 322-. |
| [10] | SONG Yue-hong, JIANG Hai-feng, PENG Su-fang, ZHAO Min. Research progress of gut microbiota in depression, anxiety and substance disorders [J]. , 2019, 39(10): 1199-. |
| [11] | GU Ting-ting, LAI Dong-mei. Research progress on the correlation between gut microbiota and obstetrics and gynecology diseases [J]. , 2018, 38(8): 967-. |
| [12] | CHU Wei-wei, XU Jie-ying, CHEN Zi-jiang, DU Yan-zhi. Effect of imblanced vaginal flora on female infertility [J]. , 2018, 38(8): 990-. |
| [13] | WANG Yin-yu1, LIU Ye1, HUANG He-feng1, 2. Roles of gut microbiota in the occurrence and development of polycystic ovary syndrome [J]. , 2018, 38(4): 454-. |
| [14] | JIA Si, YI Zheng-hui . Modified electroconvulsive therapy in the treatment of mental disorders during pregnancy#br# [J]. , 2017, 37(7): 1038-. |
| [15] | YOU Yi-jun, HAN Xiao-long, ZHENG Xiao-jiao, ZHAO Ai-hua, CHEN Tian-lu . Research progress of the bidirectional interaction between gut microbiota and brain [J]. , 2017, 37(2): 253-. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||