
上海交通大学学报(医学版) ›› 2026, Vol. 46 ›› Issue (2): 248-255.doi: 10.3969/j.issn.1674-8115.2026.02.015
• 综述 • 上一篇
收稿日期:2025-09-07
接受日期:2025-10-09
出版日期:2026-01-29
发布日期:2026-01-29
通讯作者:
程 千,主任医师,博士;电子信箱:chengqian@shsmu.edu.cn。作者简介:第一联系人:为共同第一作者(co-first authors)。
基金资助:
Lin Chao1,2, Zou Qingsong1,2, Qian Mingyang1,2, Cheng Qian2( )
)
Received:2025-09-07
Accepted:2025-10-09
Online:2026-01-29
Published:2026-01-29
Contact:
Cheng Qian, E-mail: chengqian@shsmu.edu.cn.Supported by:摘要:
骨缺损修复过程中常伴随血供不足与持续缺氧,导致细胞存活受限、血管生成受阻,并进一步抑制成骨过程。这已成为制约骨再生的重要因素。围绕这一关键瓶颈,以氧微环境调控为核心的载氧水凝胶体系逐渐成为骨组织工程领域的重要研究方向。该类体系依托水凝胶良好的生物相容性、可注射成形性及三维网络结构,通过整合过氧化物、全氟碳载氧体及酶/纳米酶等释氧模块,实现可控、可持续或微环境响应的氧气释放,并在一定程度上协同缓解氧化应激。该文系统综述了载氧水凝胶的基质材料选择、氧气来源与负载方式、释氧动力学调控策略,并从机制层面总结其在骨再生中的作用路径,包括改善局部缺氧、促进血管生成、增强成骨分化以及调节炎症反应与免疫微环境。该类体系在颅骨缺损及多种小动物骨缺损模型中可显著提高新骨形成质量与修复效率。综合现有研究证据,载氧水凝胶促进骨再生的关键不在于单纯提高氧供水平,而在于实现氧气释放强度、持续时间与骨修复阶段需求之间的精准匹配。未来研究需重点关注释氧动力学的定量调控、生物安全性及复杂病理微环境下的稳定性,以推动其向临床应用转化。
中图分类号:
林超, 邹青松, 钱名扬, 程千. 基于氧微环境调控的水凝胶体系促进骨再生的研究进展[J]. 上海交通大学学报(医学版), 2026, 46(2): 248-255.
Lin Chao, Zou Qingsong, Qian Mingyang, Cheng Qian. Advances in oxygen microenvironment-modulating hydrogel systems for bone regeneration[J]. Journal of Shanghai Jiao Tong University (Medical Science), 2026, 46(2): 248-255.
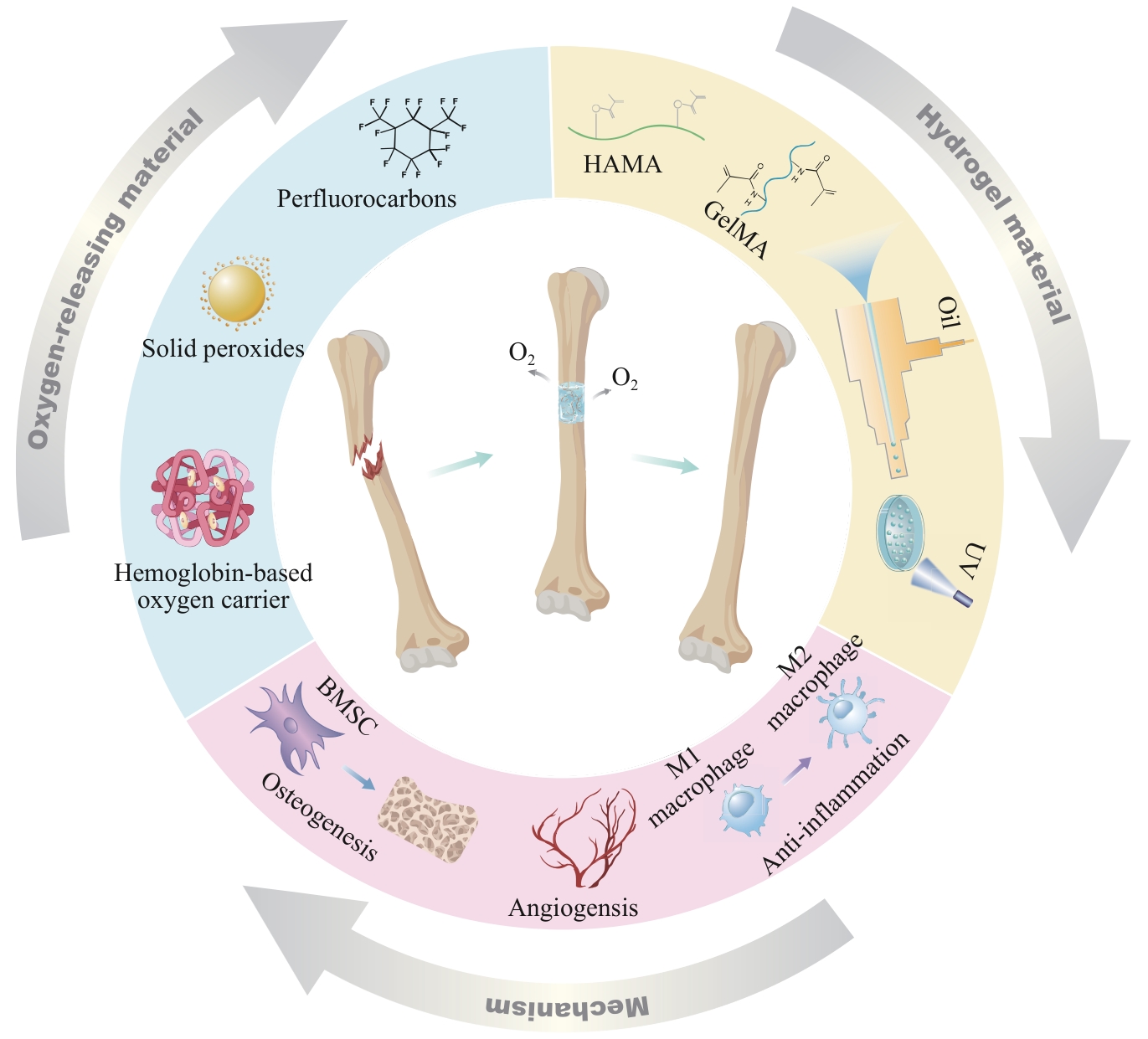
图1 基于氧微环境调控的载氧水凝胶体系设计与功能示意图Note: HAMA—hydroxyethyl methacrylate-acrylamide; GelMA—gelatin methacryloyl; BMSC—bone marrow mesenchymal stem cell.
Fig 1 Schematic illustration of the design and functions of oxygen-microenvironment-modulating oxygen-carrying hydrogel systems
| [1] | Hart N H, Newton R U, Tan J, et al. Biological basis of bone strength: anatomy, physiology and measurement[J]. J Musculoskelet Neuronal Interact, 2020, 20(3): 347-371. |
| [2] | Lin C, He J, Li J, et al. Metal coordination-based double-network microsphere scaffolds facilitate bone regeneration via oxygen-driven mitochondrial oxidative phosphorylation[J]. Chem Eng J, 2025, 512: 162233. |
| [3] | Garimella A, Ghosh S B, Bandyopadhyay-Ghosh S. Biomaterials for bone tissue engineering: achievements to date and future directions[J]. Biomed Mater, 2024, 20(1): 1-38. |
| [4] | Tang X, Zhou F, Wang S, et al. Bioinspired injectable hydrogels for bone regeneration[J]. J Adv Res, 2025, 75: 163-188. |
| [5] | Jagadale S, Damle M, Joshi M G. Bone tissue engineering: from biomaterials to clinical trials[J]. Adv Exp Med Biol, 2025, 1479: 73-115. |
| [6] | Zhao J, Sarkar N, Ren Y, et al. Engineering next-generation oxygen-generating scaffolds to enhance bone regeneration[J]. Trends Biotechnol, 2025, 43(3): 540-554. |
| [7] | Malda J, Klein T J, Upton Z. The roles of hypoxia in the in vitro engineering of tissues[J]. Tissue Eng, 2007, 13(9): 2153-2162. |
| [8] | Fu L, Zhang L, Zhang X, et al. Roles of oxygen level and hypoxia-inducible factor signaling pathway in cartilage, bone and osteochondral tissue engineering[J]. Biomed Mater, 2021, 16(2): 022006. |
| [9] | Suvarnapathaki S, Wu X, Zhang T, et al. Oxygen generating scaffolds regenerate critical size bone defects[J]. Bioact Mater, 2022, 13: 64-81. |
| [10] | Li G, Gao F, Yang D, et al. ECM-mimicking composite hydrogel for accelerated vascularized bone regeneration[J]. Bioact Mater, 2024, 42: 241-256. |
| [11] | Ding Q, Zhang S, Liu X, et al. Hydrogel tissue bioengineered scaffolds in bone repair: a review[J]. Molecules, 2023, 28(20): 7039. |
| [12] | Sun H, Xu J, Wang Y, et al. Bone microenvironment regulative hydrogels with ROS scavenging and prolonged oxygen-generating for enhancing bone repair[J]. Bioact Mater, 2023, 24: 477-496. |
| [13] | Wang C, Min S, Tian Y. Injectable and cell-laden hydrogel in the contained bone defect animal model: a systematic review[J]. Tissue Eng Regen Med, 2023, 20(6): 829-837. |
| [14] | Lukin I, Errezuma I, Garcia-Garcia P, et al. Sumecton reinforced gelatin-based scaffolds for cell-free bone regeneration[J]. Int J Biol Macromol, 2023, 249: 126023. |
| [15] | Wang C, Xu H, Liu C, et al. CaO2/gelatin oxygen slow-releasing microspheres facilitate tissue engineering efficiency for the osteonecrosis of femoral head by enhancing the angiogenesis and survival of grafted bone marrow mesenchymal stem cells[J]. Biomater Sci, 2021, 9(8): 3005-3018. |
| [16] | Zhang Y, Fang M, Zhu J, et al. Exosome-loaded hyaluronic acid hydrogel composite with oxygen-producing 3D printed polylactic acid scaffolds for bone tissue repair and regeneration[J]. Int J Biol Macromol, 2024, 274(Pt 1): 132970. |
| [17] | Ming L, Qu Y, Wang Z, et al. Small extracellular vesicles laden oxygen-releasing thermosensitive hydrogel for enhanced antibacterial therapy against anaerobe-induced periodontitis alveolar bone defect[J]. ACS Biomater Sci Eng, 2024, 10(2): 932-945. |
| [18] | Kim M J, Yoon S B, Ji H B, et al. In situ hydrogel with immobilized Mn-porphyrin for reactive oxygen species scavenging, oxygen generation, and risedronate delivery in bone defect treatment[J]. ACS Appl Mater Interfaces, 2024, 16(31): 40682-40694. |
| [19] | Lin S J, Huang C C. Strontium peroxide-loaded composite scaffolds capable of generating oxygen and modulating behaviors of osteoblasts and osteoclasts[J]. Int J Mol Sci, 2022, 23(11): 6322. |
| [20] | Xu Y, Zheng S, Tang Z, et al. Injectable, oxygen-releasing, thermosensitive hydrogel promotes vascularized bone formation with prolonged oxygen delivery and improved osteoinductivity[J]. Mater Today Bio, 2024, 29: 101267. |
| [21] | Yang Y, Wang W, Zeng Q, et al. Fabricating oxygen self-supplying 3D printed bioactive hydrogel scaffold for augmented vascularized bone regeneration[J]. Bioact Mater, 2024, 40: 227-243. |
| [22] | Augustine R, Nikolopoulos V K, Camci-Unal G. Hydrogel-impregnated self-oxygenating electrospun scaffolds for bone tissue engineering[J]. Bioengineering (Basel), 2023, 10(7): 854. |
| [23] | Huang B, Chen M, Tian J, et al. Oxygen-carrying and antibacterial fluorinated nano-hydroxyapatite incorporated hydrogels for enhanced bone regeneration[J]. Adv Healthc Mater, 2022, 11(12): e2102540. |
| [24] | Nejati S, Karimi Soflou R, Khorshidi S, et al. Development of an oxygen-releasing electroconductive in-situ crosslinkable hydrogel based on oxidized pectin and grafted gelatin for tissue engineering applications[J]. Colloids Surf B Biointerfaces, 2020, 196: 111347. |
| [25] | Rui M, Mao J, Wu H, et al. Implantable multifunctional micro-oxygen reservoir system for promoting vascular-osteogenesis via remodeling regenerative microenvironment[J]. Adv Sci (Weinh), 2025, 12(3): e2409636. |
| [26] | Gao C, Huang Y, Zhang L, et al. Self-reinforcement hydrogel with sustainable oxygen-supply for enhanced cell ingrowth and potential tissue regeneration[J]. Biomater Adv, 2022, 141: 213105. |
| [27] | Chin K, Khattak S F, Bhatia S R, et al. Hydrogel-perfluorocarbon composite scaffold promotes oxygen transport to immobilized cells[J]. Biotechnol Prog, 2008, 24(2): 358-366. |
| [28] | Kimelman-Bleich N, Pelled G, Sheyn D, et al. The use of a synthetic oxygen carrier-enriched hydrogel to enhance mesenchymal stem cell-based bone formation in vivo[J]. Biomaterials, 2009, 30(27): 4639-4648. |
| [29] | Faithfull N S. Oxygen delivery from fluorocarbon emulsions: aspects of convective and diffusive transport[J]. Biomater Artif Cells Immobilization Biotechnol, 1992, 20(2-4): 797-804. |
| [30] | Liu W, Fang Y, Xu P, et al. Cu-Fe bimetallic peroxide-based nanozyme with microenvironment-triggered cascade catalysis for synergistic hydroxyl radical, nitric oxide, and oxygen generation in trimodal wound infection therapy[J]. Mater Today Bio, 2025, 32: 101912. |
| [31] | Aleemardani M, Solouk A, Akbari S, et al. A hydrogel-fiber-hydrogel composite scaffold based on silk fibroin with the dual-delivery of oxygen and quercetin[J]. Biotechnol Bioeng, 2023, 120(1): 297-311. |
| [32] | Mohammed A A, Li S, Sang T, et al. Nanocomposite hydrogels with polymer grafted silica nanoparticles, using glucose oxidase[J]. Gels, 2023, 9(6): 486. |
| [33] | Hui Y, Mao J, Rui M, et al. Hydrogel microsphere-encapsulated bimetallic nanozyme for promoting diabetic bone regeneration via glucose consumption and ROS scavenging[J]. Adv Healthc Mater, 2024, 13(32): e2402596. |
| [34] | Mavris S M, Hansen L M. Optimization of oxygen delivery within hydrogels[J]. J Biomech Eng, 2021, 143(10): 101004. |
| [35] | Yang Z, Ren K, Chen Y, et al. Oxygen-generating hydrogels as oxygenation therapy for accelerated chronic wound healing[J]. Adv Healthc Mater, 2024, 13(3): e2302391. |
| [36] | Ke D X, Kengla C, Lee S J, et al. Release kinetics and in vitro characterization of sodium percarbonate and calcium peroxide to oxygenate bioprinted tissue models[J]. Int J Mol Sci, 2022, 23(12): 6842. |
| [37] | Haki M, Shafaei N, Moeini M. In situ gelling silk fibroin/ECM hydrogel with sustained oxygen release for neural tissue engineering applications[J]. J Biomed Mater Res A, 2025, 113(1): e37837. |
| [38] | Guan Y, Niu H, Liu Z, et al. Sustained oxygenation accelerates diabetic wound healing by promoting epithelialization and angiogenesis and decreasing inflammation[J]. Sci Adv, 2021, 7(35): eabj0153. |
| [39] | Li N, Lu X, Yang Y, et al. Calcium peroxide-based hydrogel patch with sustainable oxygenation for diabetic wound healing[J]. Adv Healthc Mater, 2024, 13(16): e2303314. |
| [40] | Wang K, Yin C, Ye X, et al. A metabolic driven bio-responsive hydrogel loading psoralen for therapy of rheumatoid arthritis[J]. Small, 2023, 19(21): e2207319. |
| [41] | Stegen S, Van Gastel N, Carmeliet G. Bringing new life to damaged bone: the importance of angiogenesis in bone repair and regeneration[J]. Bone, 2015, 70: 19-27. |
| [42] | Chen P, Liu Y, Liu W, et al. Impact of high-altitude hypoxia on bone defect repair: a review of molecular mechanisms and therapeutic implications[J]. Front Med (Lausanne), 2022, 9: 842800. |
| [43] | Zhang X, Wang H, Hao Z. A numerical bone regeneration model incorporating angiogenesis, considering oxygen-induced secretion of vascular endothelial growth factor and vascular remodeling[J]. J Biomech, 2021, 127: 110656. |
| [44] | Lv N, Hou M, Deng L, et al. A sponge-like nanofiber melatonin-loaded scaffold accelerates vascularized bone regeneration via improving mitochondrial energy metabolism[J]. Mater Today Bio, 2024, 26: 101078. |
| [45] | Yin X, Wei Y, Qin H, et al. Oxygen tension regulating hydrogels for vascularization and osteogenesis via sequential activation of HIF-1α and ERK1/2 signaling pathways in bone regeneration[J]. Biomater Adv, 2024, 161: 213893. |
| [46] | Bryniarska N, Kubiak A, Łabędź-Masłowska A, et al. Impact of developmental origin, niche mechanics and oxygen availability on osteogenic differentiation capacity of mesenchymal stem/stromal cells[J]. Acta Biochim Pol, 2019, 66(4): 491-498. |
| [47] | Hassan S, Wang T, Shi K, et al. Self-oxygenation of engineered living tissues orchestrates osteogenic commitment of mesenchymal stem cells[J]. Biomaterials, 2023, 300: 122179. |
| [48] | Farris A L, Lambrechts D, Zhou Y X, et al. 3D-printed oxygen-releasing scaffolds improve bone regeneration in mice[J]. Biomaterials, 2022, 280: 121318. |
| [49] | Lee C S, Fan J B, Hwang H S, et al. Oxygen-enriched osteoinductive nanoerythrocytes augment cell survival and osteogenic differentiation for bone regeneration[J]. Chem Mater, 2022, 34(13): 5808-5820. |
| [50] | Touri M, Moztarzadeh F, Abu Osman N A, et al. Oxygen-releasing scaffolds for accelerated bone regeneration[J]. ACS Biomater Sci Eng, 2020, 6(5): 2985-2994. |
| [51] | Volkmer E, Drosse I, Otto S, et al. Hypoxia in static and dynamic 3D culture systems for tissue engineering of bone[J]. Tissue Eng Part A, 2008, 14(8): 1331-1340. |
| [52] | Claes L, Recknagel S, Ignatius A. Fracture healing under healthy and inflammatory conditions[J]. Nat Rev Rheumatol, 2012, 8(3): 133-143. |
| [53] | Chen Q, Li J, Han F, et al. A multifunctional composite hydrogel that rescues the ROS microenvironment and guides the immune response for repair of osteoporotic bone defects[J]. Adv Funct Mater, 2022, 32(27): 2201067. |
| [54] | Xie Y, Hu C, Feng Y, et al. Osteoimmunomodulatory effects of biomaterial modification strategies on macrophage polarization and bone regeneration[J]. Regen Biomater, 2020, 7(3): 233-245. |
| [55] | Ashammakhi N, Darabi M A, Kehr N S, et al. Advances in controlled oxygen generating biomaterials for tissue engineering and regenerative therapy[J]. Biomacromolecules, 2020, 21(1): 56-72. |
| [56] | Du J, Chen T, Yu J, et al. Construction of nanohydroxyapatite/poly(sodium lipoate)-based bioactive hydrogels for cranial bone regeneration[J]. Biomacromolecules, 2025, 26(1): 705-714. |
| [57] | Wang Z, Chen T, Li X, et al. Oxygen-releasing biomaterials for regenerative medicine[J]. J Mater Chem B, 2023, 11(31): 7300-7320. |
| [1] | 黄紫晗, 黄心智. 单细胞RNA测序在骨再生研究中的应用[J]. 上海交通大学学报(医学版), 2025, 45(8): 1053-1058. |
| [2] | 鲁佳艺, 刘锦喆, 郭尚春, 陶诗聪. 纳米材料通过降低活性氧水平促进骨组织再生的研究进展[J]. 上海交通大学学报(医学版), 2025, 45(4): 487-492. |
| [3] | 何姝航, 郭尚春, 陶诗聪. 神经血管耦合在骨修复中作用的研究进展[J]. 上海交通大学学报(医学版), 2024, 44(3): 373-378. |
| [4] | 王千懿, 冉欣悦, 张沛灵, 慈政, 雷东, 周广东. 软骨脱细胞基质/丝素蛋白活性支架的构建及其软骨组织工程研究[J]. 上海交通大学学报(医学版), 2023, 43(7): 795-803. |
| [5] | 刘宏强, 陆艳青, 高宇轩, 王一云, 王传东, 张晓玲. 构建高效载体OPEI沉默TRAF6促进骨关节炎软骨再生的研究[J]. 上海交通大学学报(医学版), 2022, 42(7): 846-857. |
| [6] | 吴靖, 赵正宜, 邹多宏, 杨驰, 张志愿. 帐篷钉技术在牙槽骨重度缺损修复重建中的应用:30例临床病例回顾性分析与总结[J]. 上海交通大学学报(医学版), 2022, 42(6): 768-777. |
| [7] | 王青, 王伟, 姜达君, 贾伟涛. 钙磷涂层的JDBM镁合金多孔支架促进血管新生及骨缺损修复的效果评估[J]. 上海交通大学学报(医学版), 2021, 41(6): 732-740. |
| [8] | 李 元,史俊宇,张 枭,赖红昌. 上颌前牙区牙槽骨缺损形态学特征与引导骨再生手术效果的相关性研究[J]. 上海交通大学学报(医学版), 2020, 40(10): 1414-1419. |
| [9] | 程若昱,燕宇飞,陈皓,齐进,邓廉夫,崔文国. 双效骨诱导性的有机 - 无机水凝胶的构建及其骨再生研究[J]. 上海交通大学学报(医学版), 2018, 38(8): 900-. |
| [10] | 王德芳,乔广艳,刘 莉. 软骨细胞与复合水凝胶的生物相容性研究[J]. 上海交通大学学报(医学版), 2013, 33(11): 1465-. |
| [11] | 童文学, 向晟楠, 张 宁, 等. 大鼠关节软骨干细胞的分离培养及其特性的鉴定[J]. , 2012, 32(8): 1106-. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||